The Impact of Stress on Weight Loss and Muscle Growth
For years, stress was the missing piece that didn’t show up on lab tests, but it showed up everywhere else. In my own life and in countless client cases, I could see the same pattern: people eating “well,” moving their bodies, tracking their calories or macros, yet feeling utterly stuck with weight loss resistance and slow, frustrating muscle gains. On paper, their plans looked solid. In reality, their nervous systems were running on overdrive.
Stress isn’t just a feeling of being overwhelmed; it is a powerful biological state that quietly rewires hormones, hunger, recovery, and even where your body chooses to store fat. When it goes unchecked, it can undo weeks of careful eating and training without you ever “cheating” on your plan. In this article, the goal is to make that invisible link visible, so you can stop blaming yourself, understand what stress is really doing to your metabolism and muscles, and start using simple, realistic tools to bring your body back onside.
What Stress Actually Is (In Simple Terms)
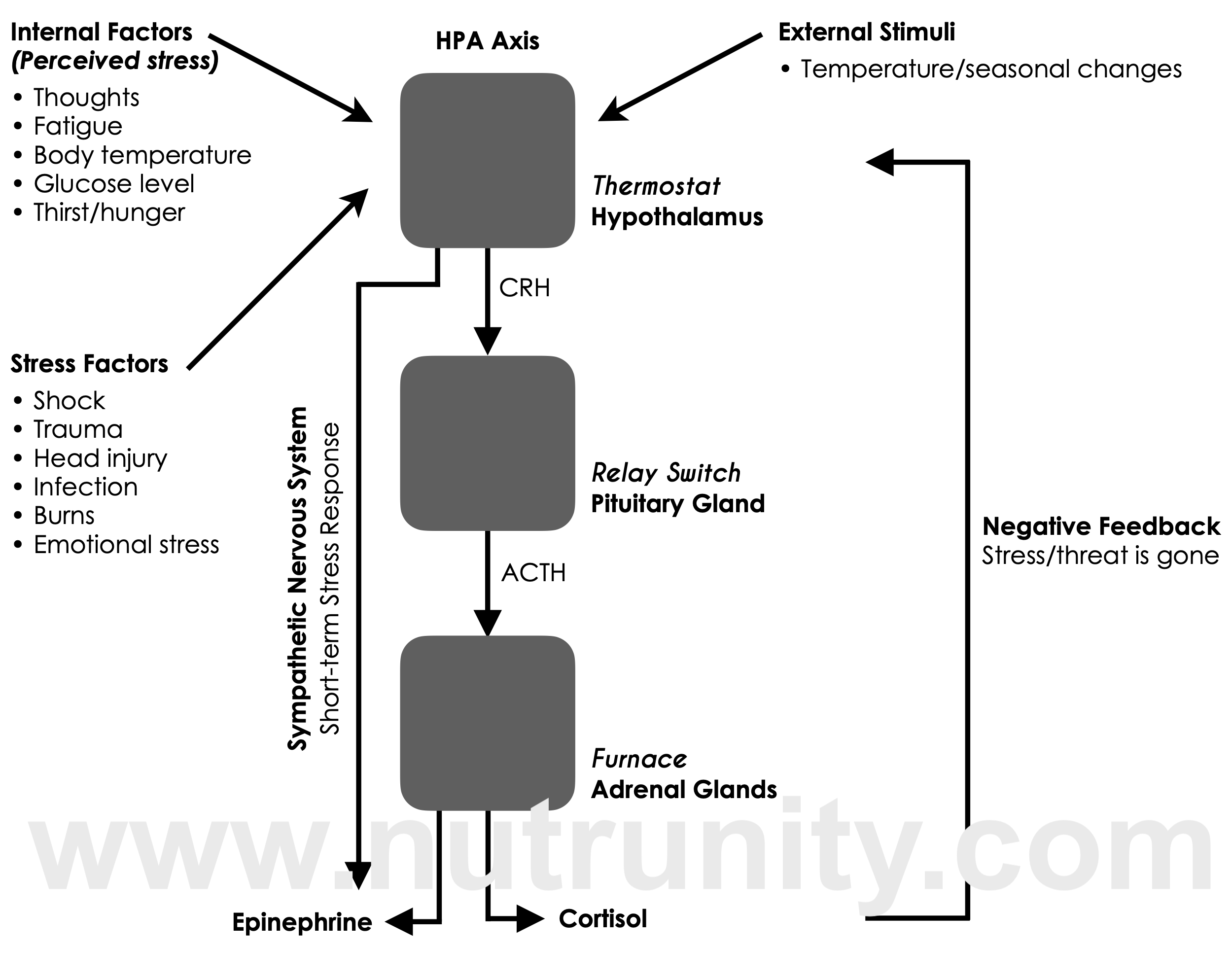
Stress is your body’s built‑in alarm system. When your brain detects a threat — real or perceived (e.g., made up, anxiety) — it activates the hypothalamic‑pituitary‑adrenal (HPA) axis, which tells your adrenal glands to release epinephrine (adrenaline) and then cortisol.
Cortisol helps you mobilise energy quickly: it raises blood sugar, heart rate and breathing; breaks down stored fuels; and switches the body into “survival mode”. This is brilliant in short bursts.
The problem is chronic stress, when that alarm stays “on” most of the time. Long‑term high cortisol and repeated HPA activation begin to change body composition (fat, muscle, and even bone mass), appetite, sleep, hormones, and how your brain reacts to food. That’s where weight loss stalls, even when you feel you’re doing everything right.
The Stress Response: HPA Axis. Illustration extracted from Energise - 30 Days to vitality. All rights reserved.
Review: What is cortisol?
Stress is part of being human. It shows up in big, dramatic moments and in the small, everyday pressures that never seem to end. Each time, your body responds automatically through the autonomic nervous system, which has two main branches: the sympathetic and the parasympathetic systems. Both work in the background to keep you alive and help you adapt to your environment.
The parasympathetic nervous system is your “rest and digest” mode. It supports digestion, elimination, immunity, healing, growth, and repair. It is the state your body needs to absorb nutrients properly, rebuild tissues (including muscle), modulate the immune system and regulate inflammation, and store energy for the future. When this system is given enough time and space to operate, your body can recover, restore, and reset.
The sympathetic nervous system is your rapid‑response mode. When it switches on, your body prepares to deal with a perceived threat through the classic “fight or flight” response. Heart rate rises, blood pressure increases, and energy is mobilised so you can act quickly. At the heart of this response is cortisol.
Cortisol is your primary, long-term response stress hormone, produced by the adrenal glands (epinephrine, or adrenaline, only lasts for so long before cortisol takes over for a sustained stress response). In short bursts, it is incredibly helpful: it raises blood sugar to give you instant fuel, sharpens your focus, and helps you respond to challenges or danger. In that sense, cortisol is not “bad”; it is a survival tool that puts your system on high alert when you need it.
The problem begins when stress is not occasional but constant. If cortisol stays elevated for long periods, the system that once protected you starts to backfire. Prolonged secretion can lead to dysregulated cortisol patterns, persistent low‑grade inflammation, and a body and mind that never entirely leave the “emergency mode.” People often experience this as ongoing tension, pain, anxiety, irritability, fatigue, and, over time, a higher risk of anxiety disorders and depression.
This chronic stress state also has a direct impact on body composition. Research has linked higher cortisol levels to a less favourable fat-to-muscle balance, typically more body fat (especially around the middle) and lower lean mass. In other words, when your stress system is constantly switched on, it becomes much harder to lose fat, protect (and build) muscle, and maintain the healthy metabolic profile you are working towards.
How Stress Makes Fat Loss Harder
1. Cortisol, Appetite, and Belly Fat
Under chronic stress, cortisol stays elevated more often than it should. Cortisol increases blood sugar and, over time, leads to insulin resistance and can push the body towards storing more fat, especially around the abdomen. Higher cortisol is associated with greater central (visceral) fat and less favourable body composition (more fat, less muscle).
Mechanisms in simple terms:
Cortisol raises blood sugar levels to provide quick energy.
Repeated surges can increase insulin levels and insulin resistance, nudging the body towards fat storage rather than fat burning.
Cortisol also interacts with hunger and reward pathways, making you more likely to crave high‑sugar, high‑fat “comfort foods” when stressed.
Over months or years, this combination can lead to weight gain or make fat loss far slower than expected, even if your diet looks “OK” on paper.
2. Emotional Eating and “Reward” Brain Circuits
Stress doesn’t just change hormones; it changes behaviour. Many people eat not only because they are hungry, but also because food temporarily soothes or distracts them. Keeping blood sugar elevated and your brain on full alert requires a tremendous amount of energy. Emotional eating and binge‑eating patterns are strongly linked to heightened HPA‑axis reactivity and stress‑related cortisol changes.
How stress feeds emotional eating:
The brain’s reward system (dopamine pathways) becomes more responsive to calorie‑dense, highly palatable foods under stress.
Eating these foods briefly calms the stress response and feels rewarding, which trains the brain to use food as a coping tool.
Over time, this can develop into a habitual pattern: stress → craving → overeating → shame → more stress.
How Stress Prevents Muscle Growth and Strength
3. Cortisol and Muscle Breakdown
Cortisol is catabolic — it breaks things down to release fuel. That includes lean muscle tissue. Chronic elevation of cortisol is linked with increased protein breakdown in muscle and reduced muscle protein synthesis. Studies show that prolonged stress and hypercortisolaemia lead to muscle atrophy via activation of proteolytic (protein‑degrading) pathways.
In plain language:
Your muscles are your body’s “protein bank.” Under chronic stress, the body withdraws more often from this bank to make glucose for the brain and vital organs.
If you are trying to build or maintain muscle, high ongoing stress levels can quietly pull you in the opposite direction, especially if your protein intake or total calorie intake is low.
If you exercise intensely to reduce stress, it can have the opposite effect, stressing your body even more.
So even with good training, gains may be slower, and losses during dieting phases may be higher when stress is not controlled.
4. Recovery, Sleep, and Training Quality
Muscle growth happens during recovery, particularly when you sleep. Chronic stress disrupts sleep onset, sleep quality, and deep sleep architecture. Poor sleep, in turn, impairs testosterone, growth hormone, and muscle protein synthesis, and increases next‑day fatigue and perceived effort.
Stress also keeps the body in a more sympathetic (“fight or flight”) state: higher muscle tension, reduced blood flow to some tissues, and increased inflammation. This can:
Make training sessions feel harder.
Increase injury risk.
Slow repair of the microscopic muscle damage that is necessary for growth.
Over time, the combination of poorer sleep, impaired recovery, and elevated cortisol creates an environment in which your body is less willing to build new muscle tissue, while you are building more fat layers. Note that you do not create new fat cells (we have a set number at birth). They are simply growing in size, and releasing high levels of oestrogens and pro-inflammatory markers as they reach full capacity, because for the body, this is not a normal situation, and it is sending signals to the brain, hoping for change; however, the inflammation is also occurring in the brain, impacting motivation, focus (think brain fog) and eating choices and patterns.
5. Stress, Bone, and Long‑Term Composition
Chronic stress affects fat and muscle, and also impacts bone. Prolonged high cortisol is associated with bone demineralisation and reduced bone mineral density, increasing fracture risk. For anyone dieting, training hard, or using weight‑loss medications, this matters: stress can quietly erode the structural foundation you rely on for movement and strength.
High caffeine intake and high blood sugar can make the blood acidic, and to buffer this, the body must release buffers from the bone matrix, such as minerals, when the available pool from the diet is insufficient. Caffeine is also a diuretic, leading to excessive mineral loss, particularly sodium and magnesium, which are essential for muscle contraction and relaxation, and nerve impulse transmission.
Other Hidden Ways Stress Disrupts Progress
6. Metabolism and “Feeling Stuck”
Experimental and observational data suggest that chronic stress and elevated cortisol are associated with a slower resting metabolic rate and unfavourable shifts in body composition. This doesn’t mean your metabolism “shuts down,” but it can make calorie deficits less effective than expected and accelerate muscle loss when dieting.
7. Motivation, Mood, and Self‑Sabotage
Stress also affects mental health. Anxiety, low mood, irritability, and fatigue are all more common when stress is high and ongoing. In that state:
Planning meals feels harder.
Saying “no” to temptations is more draining.
A missed workout is more likely to turn into a missed week.
None of this is laziness. It is what happens when your emotional bandwidth is exhausted just getting through the day, and you waste too much energy sustaining the stress response.
Practical, Low‑Cost Ways to Lower Stress (That Fit Real Life)
You cannot erase stress from life, but you can turn down its impact on your body and mind. The goal is not to become perfectly calm; it is to give your nervous system regular signals of safety so it doesn’t have to live in survival mode.
1. Use Simple Breathing as a “Reset Button” (essential and non-negotiable!)
There is no way around it. We have forgotten to breathe correctly, and when stressed, the breath is shallower and faster, leading to a faster heart rate. Conscious breathing unsettles the brain, so it must reset because it is not expecting you to change your breathing when danger is imminent. If you breathe deeply, the brain begins to think you are safe and switches out of survival mode. Slow, diaphragmatic breathing is one of the fastest ways to shift your nervous system out of fight‑or‑flight and into a more parasympathetic (“rest and digest”) state.
Try this:
Inhale gently through your nose for 4 seconds.
Pause for 1–2 seconds.
Exhale slowly through pursed lips for 6–8 seconds.
Repeat for 2–5 minutes, 1–3 times per day, or whenever you feel “amped up.”
If it sounds too complicated, try box breathing':
Inhale gently through your nose for 4-8 seconds (whichever feels comfortable for you)
Pause for 4-8 seconds.
Exhale slowly through pursed lips for 4-8 seconds.
Repeat for 2–5 minutes, or until you feel in control of your thoughts. When doing this exercise, using positive thoughts is even more powerful.
This can be done at your desk, in the bathroom, or before sleep, no equipment required.
2. Prioritise “Anchor” Sleep Habits
You may not be able to get perfect sleep, but a couple of anchors make a real difference:
Aim for a fairly consistent bedtime and wake time, even on weekends.
Create a 20–30-minute “wind‑down” routine: dim the lights, turn screens off or on to night mode, do gentle stretching, read, or take a bath. Create a routine that tells the brain it is time to wind down and prepare for sleep, so it can start producing melatonin and allow you to sleep properly and reach deep sleep for more extended periods. This is not possible when cortisol levels are high because cortisol opposes melatonin. Remember that melatonin is a very powerful antioxidant, allowing for healing and repair. Without proper sleep, this does not happen, nor can the glymphatic system clear toxins and metabolic waste from the brain, a leading cause of neurodegeneration over the long term.
Good sleep helps normalise cortisol patterns, supports appetite hormones like leptin and ghrelin, and improves insulin sensitivity, all of which support fat loss and muscle recovery.
3. Move Your Body for Stress Relief, Not Just Calories
Physical activity is a powerful stress‑reliever and helps lower baseline cortisol over time. You don’t need long gym sessions; small, regular bouts are enough to help. Plus, it is free and the most underused antidepressant.
Options:
10–15 minutes of brisk walking once or twice a day.
A simple home strength circuit 2–3 times per week (squats to a chair, wall push‑ups, lunges or step‑ups, light dumbbells or resistance bands).
Gentle yoga or stretching on rest days. Aim to stretch before bed if you feel muscle tension. It is also great in the morning to help you focus on your body rather than the day ahead and the stress that comes with it.
This not only supports body composition but also gives you a constructive outlet for tension and improves your mood.
Exercise and stress: Get moving to lower stress
Exercise is one of the most reliable, low‑cost ways to turn down your body's stress response. Almost any movement you enjoy, from walking and dancing to swimming or yoga, can help.
When you move, your body releases chemicals called endorphins and other “feel‑good” neurotransmitters, which can lift your mood and reduce the perception of pain and discomfort. Exercise also helps counter some of the physical effects of chronic stress by lowering resting heart rate and blood pressure, supporting cardiovascular and immune health, and improving sleep quality. In many people, regular activity eases symptoms of mild anxiety and depression and makes everyday challenges feel more manageable.
You don’t need long gym sessions to benefit. Public health guidelines suggest aiming for at least 150 minutes of moderate aerobic activity (such as brisk walking, cycling, or gentle swimming) or 75 minutes of vigorous activity (such as running or fast lap swimming) per week, plus strength training for major muscle groups on at least 2 days. If that feels like too much right now, start smaller: several 5–10-minute walks or movement “snacks” spread throughout the day still help, and they add up. Think walking up the escalator instead of staring at your phone or walking up the stairs instead of taking the lift to reach the first or second floor. Adapt effort to your abilities.
The best stress‑relieving exercise is the one you’ll actually do. That could be walking the dog, following a short video at home, gardening, climbing stairs, or a weekly class. Put movement into your diary like any other appointment, vary it when you get bored, and, if possible, involve a friend to boost motivation and enjoyment. Over time, being active becomes less of a chore and more of a built‑in way to clear your head and support your nervous system.
4. Create Tiny, Realistic Food Boundaries Around Stress
You can’t remove every emotional trigger, but you can make it easier for your body to cope:
Don’t let yourself get too hungry: aim for regular meals or planned snacks with protein and fibre to keep blood sugar steadier and reduce stress‑driven binges.
Keep some “safety foods” at home; nutritious options you genuinely enjoy and can prepare quickly, so you’re less reliant on last‑minute, ultra‑processed comfort foods.
If you notice repeated stress‑eating, start with awareness rather than judgement: name the feeling (“I’m overwhelmed / lonely / exhausted”) before you decide what to do. That pause alone begins to loosen the stress–food loop.
5. Practise 5‑Minute “Decompression Windows”
If your day is non‑stop, you may need micro‑breaks more than hour‑long rituals. Try:
5 minutes between tasks with no screens: look out of a window, stand up, stretch, breathe.
A short walk around the block before you enter the house after work, to “change gears.”
Set a timer 2–3 times a day to check in: unclench your jaw, drop your shoulders, exhale fully, or go to the fountain for a glass of water. That short walk may help you think clearly, without anyone noticing.
These tiny windows prevent stress from accumulating unchecked and make it easier to access calm later.
6. Strengthen Social Support (Even in Small Ways)
Feeling supported reduces perceived stress and improves resilience. You do not need a huge social life to benefit:
Send one honest message a week to a friend or family member.
Schedule a regular call or walk with one person you trust.
Consider a group class, community activity, or online support group related to your goals (fitness, nutrition, stress, or a hobby you enjoy).
Knowing you’re not doing this alone makes it easier to maintain new habits and reduces reliance on food or overtraining as coping mechanisms.
Bringing It All Together
Stress is not just an annoying feeling; it is a physiological state that alters hormones, appetite, body composition, recovery, and behaviour. Chronic stress can:
Increase belly fat and slow fat loss.
Drive emotional eating and cravings.
Erode muscle and bone.
Disrupt sleep and recovery.
Drain the motivation and clarity you need to change.
None of this means your goals are out of reach. It means that willpower and macros are only part of the story. By weaving in even a few simple stress‑reduction habits (e.g., breathing, better sleep anchors, stress‑relieving movement, supportive food choices, micro‑breaks, and connection), you create a body and brain that can respond to your training and nutrition efforts, and help you lose weight naturally.
Progress may still be gradual, and life will still be messy. But you will no longer be fighting your own biology at every step. Instead, you’ll be working with it, and that’s where sustainable fat loss, stronger muscles, and boundless vitality become possible and a reality over the long term.
Must Read:
Sanchez, O. (2021). Energise -30 Days to Vitality. Nutrunity Publishing. London.
Sanchez, O. (2023). Detox before Energise. Nutrunity Publishing. London.
References
Adam, TC. Epel, ES. (2007). Stress, eating and the reward system. Physiology & Behavior. 91(4), pp. 449-458. doi:10.1016/j.physbeh.2007.04.011
Agarwal, V. Gupta, A. Chaudhary, R. (2025). Elucidating the potential mechanism and therapeutic targets of chronic stress-induced muscle atrophy. International Immunopharmacology. 162, 115118. doi:10.1016/j.intimp.2025.115118
Bose, M. Oliván, B. Laferrère, B. (2009). Stress and obesity: The role of the hypothalamic-pituitary-adrenal axis in metabolic disease. Current Opinions in Endocrinology, Diabetes and Obesity. 16(5), pp. 340-346. doi:10.1097/MED.0b013e32832fa137
Chang, RS. Cerit, H. Hye, T. et al. (2022). Stress-induced alterations in HPA-axis reactivity and mesolimbic reward activation in individuals with emotional eating. Appetite. 168, 105707. doi:10.1016/j.appet.2021.105707
Cvijetic, S. Keser, I. Jurasović, J. et al. (2022). Diurnal salivary cortisol in relation to body composition and heart rate variability in young adults. Frontiers in Endocrinology (Lausanne). 13, 831831. doi:10.3389/fendo.2022.831831
Hewagalamulage, SD. Lee, TK. Clarke, IJ. et al. (2016). Stress, cortisol, and obesity: A role for cortisol responsiveness in identifying individuals prone to obesity. Domestic Animal Endocrinology. 56(Suppl.), S112-120. doi:10.1016/j.domaniend.2016.03.004
Incollingo Rodriguez AC. Epel, ES. White, ML. et al. (2015). Hypothalamic-pituitary-adrenal axis dysregulation and cortisol activity in obesity: A systematic review. Psychoneuroendocrinology. 62, pp. 301-318. doi:10.1016/j.psyneuen.2015.08.014
Kukić, F. Heinrich, KM. (2025). Editorial: Physical activity behavior, obesity, and stress as crucial sources of health issues in stressful occupations, volume II. Frontiers in Endocrinology (Sec. Obesity). doi:10.3389/fendo.2025.1742390
Maruszczak, K. Kasperek, W. Kustra, K. et al. (2025). Exploring the science of shape: How physical activity, sleep, and stress affect body composition. Healthcare (Basel). 13(8), 949. doi:10.3390/healthcare13080949
Segal, Y. Gunturu, S. (2025). Psychological issues associated with obesity. [Updated 2024]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK603747
Thau, L. Gandhi, J. Sharma, S. (2025). Physiology, Cortisol. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538239/
Toussaint, L. Nguyen, QA. Roettger, C. et al. (2021). Effectiveness of progressive muscle relaxation, deep breathing, and guided imagery in promoting psychological and physiological states of relaxation. Evidence-Based Complementary and Alternative Medicine. 2021, 5924040. doi:10.1155/2021/5924040
van Dalfsen, JH. Markus, CR. (2018). The influence of sleep on human hypothalamic-pituitary-adrenal (HPA) axis reactivity: A systematic review. Sleep Medicine Reviews. 39, pp. 187-194. doi:10.1016/j.smrv.2017.10.002
Vargas, I. Lopez-Duran, N. (2017). Investigating the effect of acute sleep deprivation on hypothalamic-pituitary-adrenal-axis response to a psychosocial stressor. Psychoneuroendocrinology. 79, pp. 1-8. doi:10.1016/j.psyneuen.2017.01.030
Worthen, M. Cash, E. (2025). Stress Management. [Updated 2023]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513300
Yau, YH. Potenza, MN. (2013). Stress and eating behaviors. Minerva Endocrinologica. 38(3), pp. 255-267.