Type 5 Diabetes (Malnutrition-Related Diabetes): A Comprehensive Overview
The world of diabetes has just become more complicated. In a landmark development, the International Diabetes Federation (IDF) has officially recognised a new form of diabetes: Type 5.
If your immediate thought is, “Hang on, weren’t there only two types?”, you’re certainly not alone.
In truth, diabetes isn’t a simple two-option diagnosis. Rather, it’s a broad and evolving spectrum of conditions that affect millions of people in different ways. From genetic forms to hormone-related variants and even diabetes caused by malnutrition, the condition encompasses more than a dozen recognised types, each with distinct causes, mechanisms, and treatments.
This guide will help you make sense of the expanding diabetes landscape, from the well-known to the rare and newly recognised. Whether you’re living with diabetes, supporting someone who is, or simply looking to learn more, here’s what you need to know, no medical degree required.
What forms of diabetes are there?
What Is Diabetes?
Diabetes is a complex group of chronic metabolic disorders characterised by elevated blood sugar levels. This condition arises when the body either produces too little insulin, a vital hormone that enables cells to absorb and use glucose, or cannot use insulin effectively. Insulin’s regulation of glucose is central to maintaining health, and its failure can result in long-term damage to the blood vessels, nerves, heart, kidneys, and eyes.
While most people are acquainted with the more common types, Type 1, Type 2, and gestational diabetes (developing during pregnancy), there is a broader spectrum of diabetes, including several lesser-known or emerging forms. Each type has distinct causes, symptoms, and treatment approaches. Understanding this full range is crucial not only for proper diagnosis and care but also for the development of effective global strategies to prevent disability and premature death.
— The Global Burden of Diabetes in 2025
Today, diabetes represents one of the most urgent and fastest-growing public health challenges worldwide.
Prevalence:
As of 2025, an estimated 589 million adults (20–79 years) are living with diabetes globally, about 1 in every 9 adults.
Growth: This number is expected to soar, reaching 853 million by 2050 if current trends continue.
Geography: Over 80% of adults with diabetes live in low- and middle-income countries, where the incidence and the treatment gaps are most significant.
According to the CDC, from August 2021 to August 2023, the prevalence of total diabetes was 15.8% (nearly 5% of which were undiagnosed) among the total adult population. In the UK, the NHS identifies that every year, over half a million people are found to have insulin resistance (pre-diabetics). Nearly 4 million Britons were diagnosed with Type 2 Diabetes in 2021 (that’s a prevalence of 7.8% in the general population).
“Our data shows that almost 4.6 million people in the UK live with diabetes diagnoses. Additionally, nearly 1.3 million people could be living with type 2 diabetes who are yet to be diagnosed.”
Undiagnosed Cases: Globally, 252 million people are believed to be living with undiagnosed diabetes, placing them at heightened risk for serious complications. Most are not diagnosed until after developing advanced health problems.
Childhood and Youth Impact: There are approximately 1.8 million children and young adults under 20 diagnosed with Type 1 diabetes, and increasing evidence suggests earlier onset of other forms in younger populations.
Deaths: In 2024, diabetes was responsible for over 3.4 million deaths annually worldwide; an enormous toll reflecting the direct and indirect consequences of the disease.
Healthcare Costs: In 2024, global diabetes-related expenditures surpassed USD 1 trillion for the first time, exposing the immense economic and social burden from treatment, complications, and lost productivity.
“As of 2025, an estimated 589 million adults (20–79 years) are living with diabetes globally, about 1 in every 9 adults. This number is expected to soar, reaching 853 million by 2050 if current trends continue.”
— Regional Trends and Future Risks
Diabetes is rising most rapidly in regions struggling with poverty, food insecurity, and limited access to healthcare. Countries in South-East Asia, Africa, and the Middle East are projected to see the steepest increases, a trend driven by urbanisation, changing diets, sedentary lifestyles, and demographic shifts. For example, Africa is expected to have a 142% increase in diabetes cases by 2050, and South-East Asia a 73% rise.
The impact is particularly devastating in low-resource settings, where fewer than 4 in 10 adults with diabetes have access to ongoing medical treatment or glucose-lowering medications. Diabetes-related complications, including amputations, heart disease, kidney failure, and blindness, are more common where care is inaccessible or delayed.
— Why Action Matters
Diabetes now ranks among the leading causes of death and disability worldwide, driving up healthcare costs and threatening development in vulnerable economies. Its burden has quadrupled globally since 1990 due to population growth, urbanisation, increased life expectancy, obesity, and lifestyle changes.
With so many living undiagnosed, diabetes is frequently a “silent” threat, only recognised after significant — and sometimes irreversible — complications occur.
“With over 4 in every 10 people with diabetes not yet diagnosed, governments must prioritise screening, early diagnosis, and education. Addressing the rising tide of diabetes will demand collaboration across multiple sectors and disciplines. Governments, the healthcare sector, education, technology and the private sectors all have a role to play. The consequences of ignoring or not paying sufficient attention to the diabetes challenge are too significant. Inaction in the face of this pandemic is not an option.”
How Type 5 Diabetes Came to Light
In April 2025, the International Diabetes Federation (IDF) made a momentous announcement that has reshaped the medical community’s understanding of diabetes. For the first time in decades, Type 5 diabetes was officially recognised as a distinct form of the disease. This monumental decision brought to light a health crisis that had long been hidden, one affecting millions, primarily in poor regions of the world, who had suffered in silence due to misdiagnosis and a lack of targeted treatments. Now identified as a unique condition tied to profound early-life malnutrition, Type 5 diabetes demands urgent global attention.
Unlike Types 1 and 2 diabetes, Type 5 is not linked to autoimmune responses or insulin resistance caused by obesity. Instead, it emerges from severe protein and nutrient deficiencies during critical periods of childhood development. These early nutritional insults stunt the growth and function of the pancreas and related metabolic systems, leaving individuals much more vulnerable to chronic high blood sugar later in adolescence or young adulthood. What makes Type 5 particularly perplexing for clinicians is how its symptoms mirror those of other diabetic types: increased thirst, frequent urination, fatigue, and unexplained weight loss. Yet, the patients affected are strikingly lean and often live in low-income settings, making standard diabetes treatments less effective and the condition easy to overlook.
This silent epidemic affects an estimated 20 to 25 million people worldwide, predominantly concentrated in South Asia and Sub-Saharan Africa. For decades, many of these individuals have been misclassified as having atypical Type 1 or Type 2 diabetes. The consequences have been dire; many young adults face early death or debilitating complications without ever understanding the root cause of their illness. Malnutrition, far beyond its obvious toll on children’s physical growth, also rewires their metabolic programming in ways that set the stage for irreversible health problems.
The delayed recognition of Type 5 diabetes reflects deep systemic failures within global health. For years, malnutrition was often relegated to the realm of charity rather than urgent medical research, while wealthier countries’ concerns about obesity and autoimmunity dominated scientific inquiry. Resource-poor regions, where the disease is most prevalent, often lack robust health infrastructure, and many cases go undetected and unreported. Stigma and assumptions that diabetes had to involve excess weight further blinded clinicians to this form of the disease. Funding priorities overlooked malnutrition-related illnesses, perpetuating the invisibility of millions suffering quietly and dying too early.
With official recognition comes opportunity. The global health community must act decisively. New diagnostic guidelines are being developed to help healthcare workers differentiate Type 5 diabetes from other variants early and accurately. Treatment protocols are pivoting to incorporate nutritional rehabilitation alongside medical management. Governments and aid organisations are challenged to prioritise sustainable food security initiatives as fundamental to preventing this disease, transforming social support programmes into powerful health interventions. The implications stretch well beyond diabetes care, emphasising how investments in childhood nutrition yield long-term dividends in public health.
Experts highlight both the promise and the challenges ahead. Dr. Lindiwe Ngugi, a renowned endocrinologist, describes Type 5 diabetes as a wake-up call for global medicine to confront the devastating metabolic consequences of malnutrition. Sanjay Patel, a policy advisor, stresses that this recognition opens doors for specialised care that was previously impossible, but warns that sustained political will is critical for impact. Today’s breakthroughs offer hope, yet significant barriers remain in reaching the most vulnerable populations and scaling life-saving programs.
The arrival of Type 5 diabetes as a formally classified disease is not just a medical event but a pivotal moment of moral reckoning. For millions around the globe, it affirms that their suffering is real and demands tailored solutions. The world now has a choice: to mobilise with urgency and compassion or to allow this silent epidemic to continue claiming young lives unseen. Addressing Type 5 diabetes means confronting poverty, food insecurity, and health inequities head-on, offering a new path to a healthier, more just future.
Diagnosis and Metabolic Profile
Type 5 diabetes is characterised by severe insulin deficiency without insulin resistance. Unlike Type 2 diabetes, many patients can manage their condition with oral medications rather than insulin injections, which is particularly beneficial in resource-limited settings. Accurate diagnosis requires recognising the distinct metabolic and clinical profile, including low BMI and a history of undernutrition.
The formal recognition of Type 5 diabetes by the IDF marks a significant milestone in global diabetes care. It aims to:
Reduce misdiagnoses that have long affected millions
Promote personalised, effective, and cost-efficient treatment strategies
Prioritise care and resources in low-income regions where the disease burden is highest
The IDF has established a working group dedicated to creating diagnostic criteria and treatment guidelines focused on equity, scientific rigour, and saving lives.
Treatment
Replace lost insulin function
Restore nutritional balance
Prevent complications
Minimise treatment burden in low-resource areas
— Nutritional Rehabilitation
High-protein, energy-dense diets to rebuild metabolic capacity
Micronutrient supplementation (zinc, iron, vitamins A, D, and B-complex)
Pancreatic enzyme support, if exocrine function is compromised
Oral nutrient support in cases of severe undernutrition
— Monitoring and Follow-up
Routine blood glucose monitoring
Weight and nutrition tracking (e.g., monthly BMI reviews)
Annual screening for complications: kidneys, eyes, nerves
Psychological and social support, especially in adolescence
What happens if it’s misdiagnosed?
If patients with Type 5 diabetes are treated as though they have Type 1:
They may be given lifelong insulin unnecessarily
The risk of hypoglycaemia increases in patients with low caloric intake
Treatment costs rise (a significant barrier in resource-limited settings)
Nutritional aspects go ignored, worsening long-term prognosis
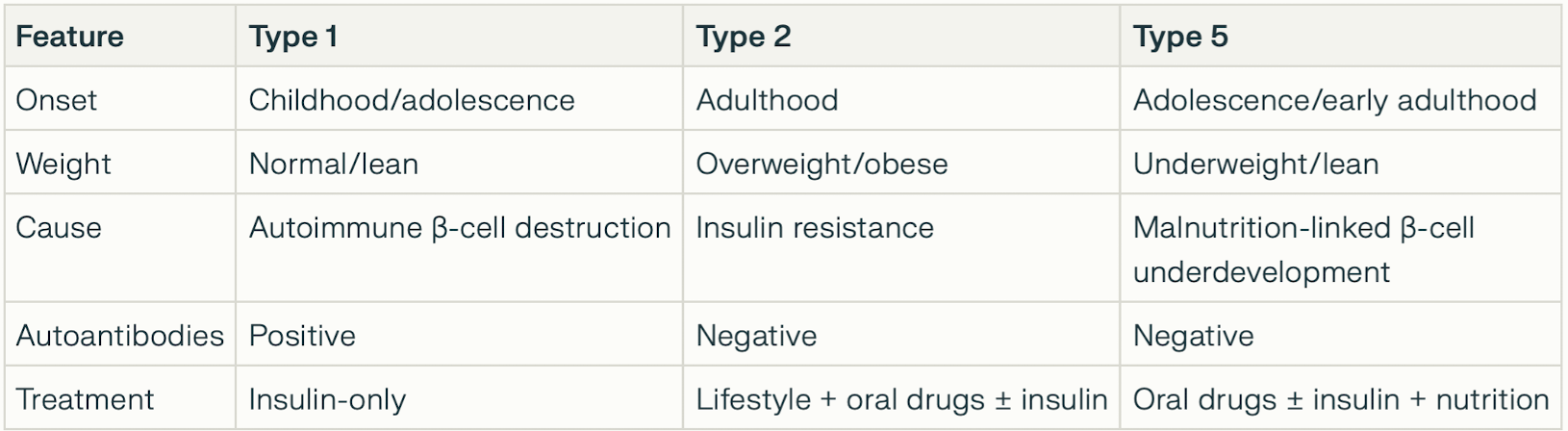
Differences between Type 1, Type 2 and Type 5 diabetes
Sources:
International Diabetes Federation
https://diabetesatlas.org/media/uploads/2025/04/2025-IDF-Diabetes-Atlas-Press-Release-FINAL-Embargo.pdf
https://idf.org/news/new-type-5-diabetes-working-group
NHS UK
World Health Organization (WHO)
References:
Boyko, EJ. Ong, KL. Duncan, BB. (2025). Worldwide trends in diabetes prevalence: The NCD-RisC study. Lancet. 406(10499), pp. 131-132. doi:10.1016/S0140-6736(25)01079-7
CDC. (2025). Prevalence of Total, Diagnosed, and Undiagnosed Diabetes in Adults: United States, August 2021–August 2023. Available at: https://www.cdc.gov/nchs/products/databriefs/db516.htm
Guariguata, L. Sobers, N. (2024). Rising diabetes, lagging treatment, and the need for better systems. Lancet. 404(10467), pp. 2026-2028. doi:10.1016/S0140-6736(24)02422-X
International Diabetes Federation. (2025). Diabetes Atlas. 11th Edition. Available at: https://diabetesatlas.org/media/uploads/sites/3/2025/04/IDF_Atlas_11th_Edition_2025.pdf
Jebasingh, F. Thomas, N. (2025). Type 5 Diabetes - The rejuvenated spirit from a ghost of the past. Indian Journal of Endocrinology and Metabolism. 29(3), pp. 249-252. doi:10.4103/ijem.ijem_404_25
Lipscombe L, Dasgupta K, Shah B. Worldwide trends in diabetes prevalence: the NCD-RisC study. Lancet. 2025 Jul 12;406(10499):132-133. doi: 10.1016/S0140-6736(25)01080-3. PMID: 40651817.
NCD Risk Factor Collaboration (NCD-RisC). (2024). Worldwide trends in diabetes prevalence and treatment from 1990 to 2022: a pooled analysis of 1108 population-representative studies with 141 million participants. Lancet. 404(10467), pp2077-2093. doi:10.1016/S0140-6736(24)02317-1
Prajitno, JH. Sutanto, H. (2025). Type 5 diabetes as a growing malnutrition driven health crisis in low and middle income countries. Journal of diabetes and metabolic disorders. 24, 162. doi:10.1007/s40200-025-01674-w
Selim, S. (2025). Type 5 Diabetes Mellitus: Global recognition of a previously overlooked subtype. Bangladesh Journal of Endocrinology and Metabolism. 4(2), pp. 59-60. doi:10.4103/bjem.bjem_13_25
Zhou, B. Gregg, EW. Danaei, G. et al. (2025). NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in diabetes prevalence: the NCD-RisC study - Authors’ reply. Lancet. 406(10499), pp. 133-134. doi: 10.1016/S0140-6736(25)01085-2