From Gut Dysbiosis to Neurodegeneration: The Final Link in Obesity-Cognitive Difficulties
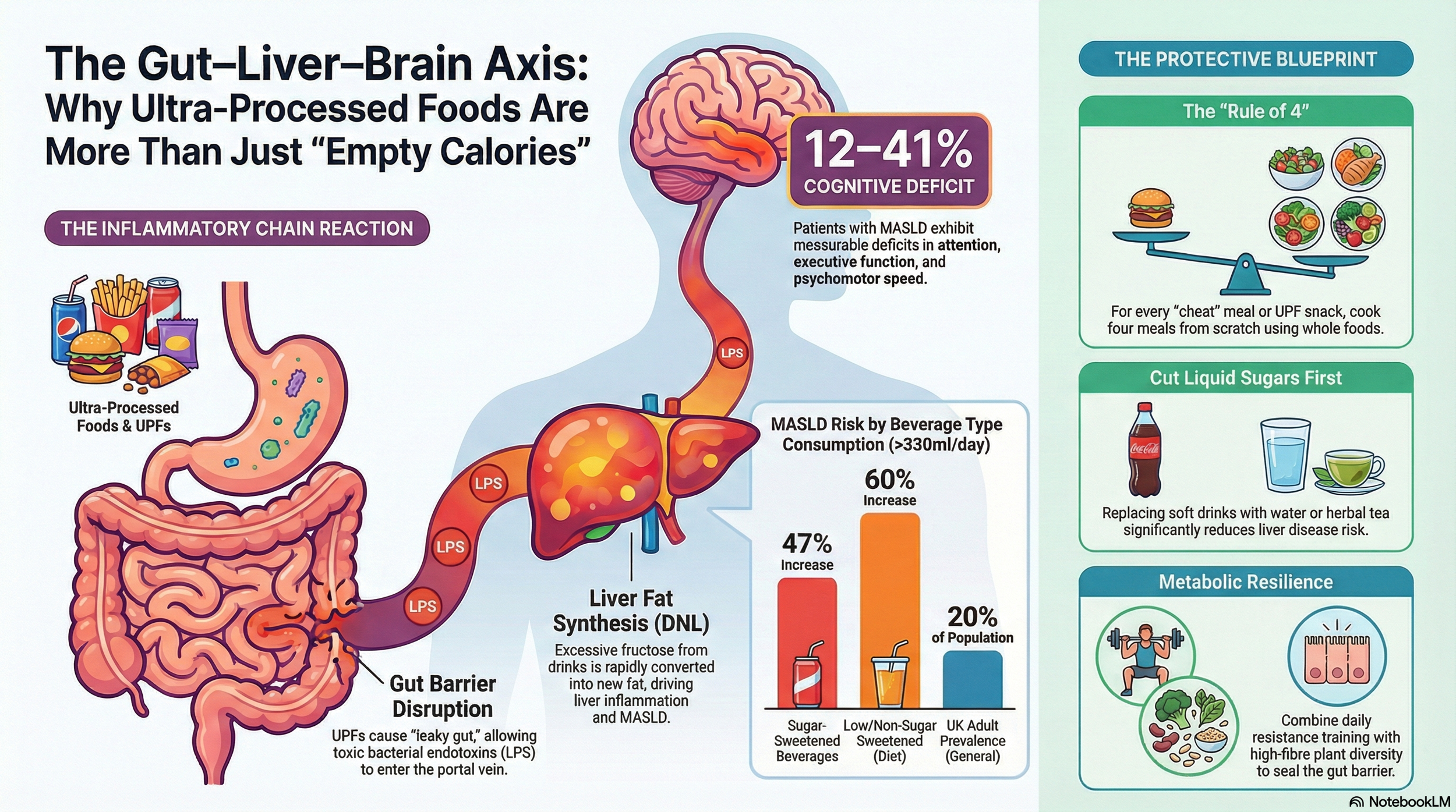
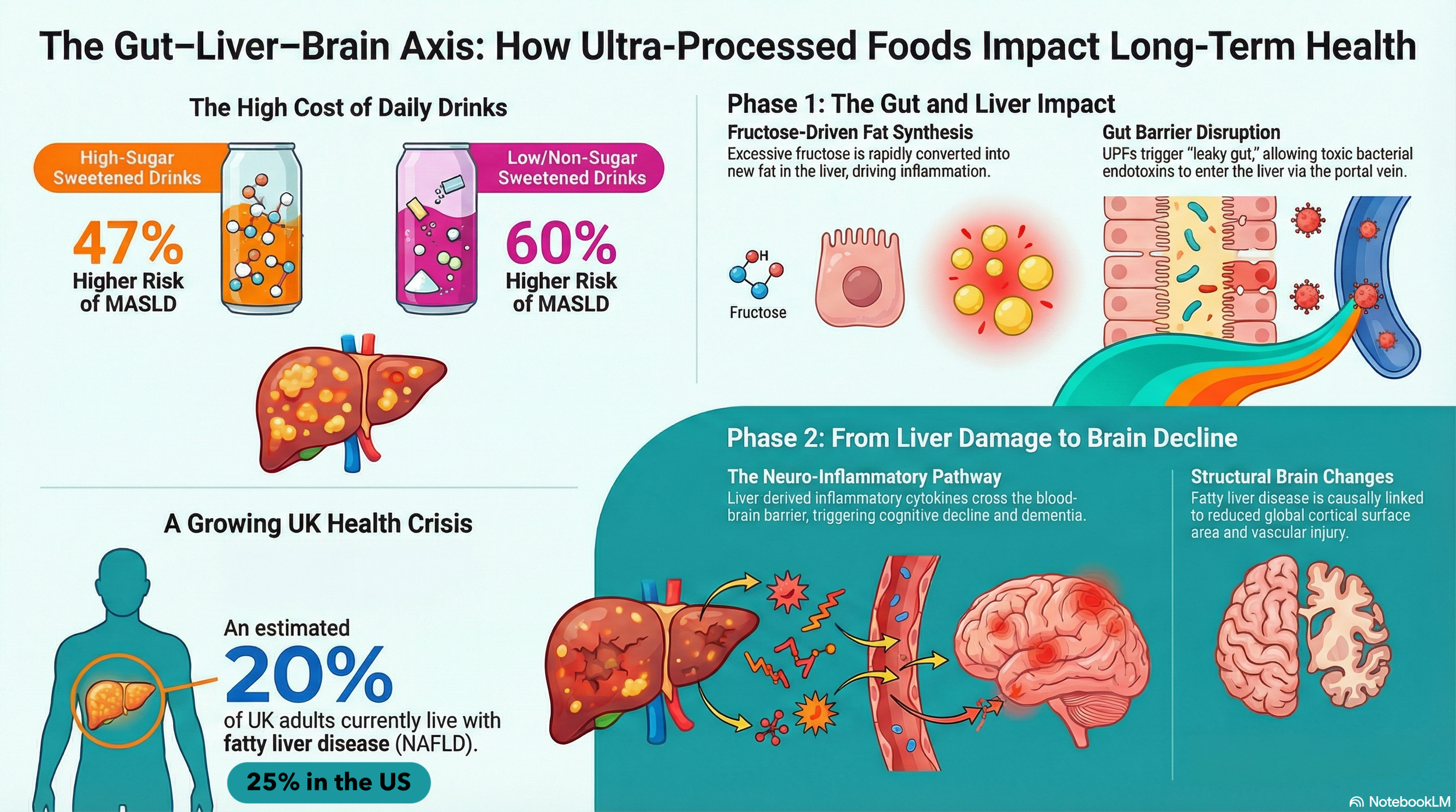
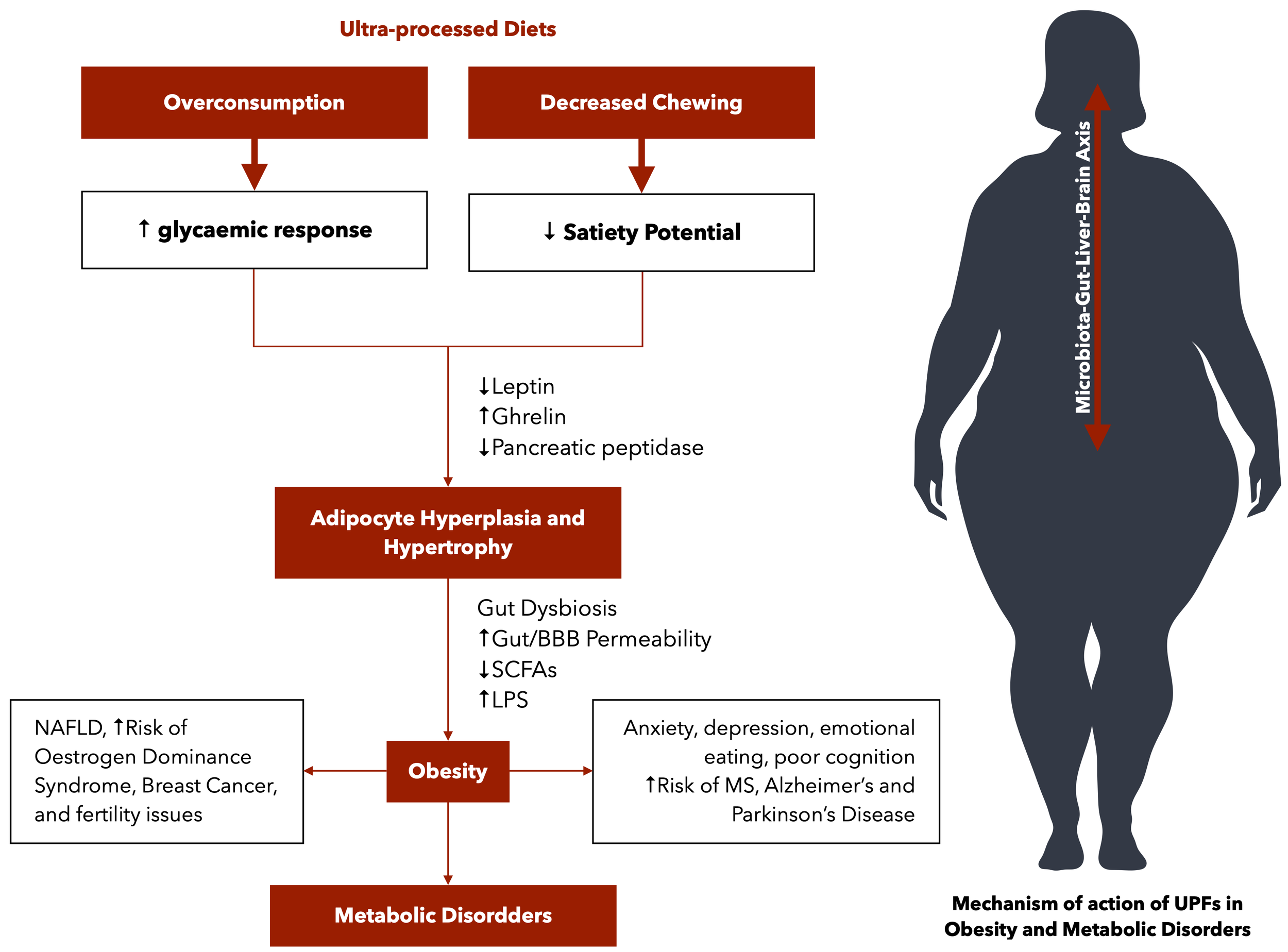
The convergence of metabolic dysfunction, gut dysbiosis, and neuroinflammation forms a deadly triad that accelerates neurodegenerative diseases like Alzheimer’s and multiple sclerosis (MS). Ultra-processed diets act as the catalyst, creating a perfect storm and damaging the gut, liver, and brain.
Alzheimer’s Disease: The Gut-Brain Axis Collapse
Emerging evidence positions Alzheimer’s as a metabolic disorder with roots in gut dysbiosis and systemic inflammation. UPFs disrupt gut microbiota diversity, reducing beneficial Bifidobacterium and Lactobacillus strains while promoting pro-inflammatory Proteobacteria. This dysbiosis elevates circulating lipopolysaccharides (LPS) and decreases short-chain fatty acids (SCFAs), which are critical for maintaining the gut lining and blood-brain barrier (BBB) integrity and suppressing neuroinflammation.
Microglial cells and astrocytes, activated by LPS and cytokines (IL-6, IL-1α), enter a perpetual state of inflammation, releasing reactive oxygen species (ROS - free radicals) and amyloid-beta plaques. Hippocampal neurones, essential for memory, are particularly vulnerable to this assault, showing 30% reduced synaptic plasticity in animal models fed UPFs. Human studies confirm that UPF-heavy diets correlate with 2.3x higher Alzheimer’s risk, driven by chronic neuroinflammation and BBB leakage.
The LPS-Liver-Brain Axis
UPFs rich in trans fats and emulsifiers provoke low-grade inflammation and intestinal permeability, allowing LPS (endotoxins) to flood circulation. These endotoxins trigger hepatic inflammation, contributing to non-alcoholic fatty liver disease (NAFLD) — present in 67% of obese individuals. The liver’s compromised state amplifies systemic inflammation, marked by:
45% higher IL-6
32% elevated triglycerides
28% increased postprandial insulin
This inflammatory cocktail degrades tight junction proteins in the BBB, permitting peripheral immune cells and cytokines to infiltrate the brain. Once inside, LPS binds to Toll-like receptors on microglia and astrocytes, triggering a self-sustaining loop of ROS production, neuronal damage, and amyloid deposition.
Multiple Sclerosis: The Role of SCFAs
The gut microbiome’s role in autoimmune demyelination is exemplified in MS. UPFs deplete SCFA-producing bacteria (Faecalibacterium, Roseburia), slashing propionic acid levels by 40% — a key regulator of regulatory T-cells (Tregs). In groundbreaking work by Prof. Aiden Haghikia’s team at Ruhr-University Bochum, MS patients showed:
55% lower faecal propionate vs. controls
3x higher Th17 cell activity, driving neuroinflammation
Impaired oligodendrocyte maturation, worsening demyelination
SCFAs like propionate can restore gut-brain communication, suppressing IL-17 and promoting Treg differentiation. UPFs disrupt this balance, creating an environment ripe for autoimmune attacks on myelin. Biofilms are also suspected in MS, shedding new light on systemic inflammation triggered by chronic infections.
How Ultra-Processed Diets Fuel Emotional Eating and Mental Health Decline
The relationship between ultra-processed diets, obesity, and mental health is not just a correlation — it’s a self-perpetuating storm. Emerging research reveals that UPFs don’t merely affect mood; they trap individuals in a biochemical and psychological loop where anxiety, depression, and disordered eating reinforce one another.
The Mood-Food Feedback Loop
A 2022 meta-analysis of 385,541 individuals found that high UPF consumption increases the odds of depression by 44% and anxiety by 48%. But why does this happen? The answer lies in three intersecting pathways:
Neurochemical Hijacking
UPFs — packed with refined sugars, trans fats, and artificial additives — flood the brain with dopamine, creating short-lived euphoria. Over time, this blunts the brain’s natural reward circuitry, requiring larger quantities to achieve the same “high.” Simultaneously, these foods deplete serotonin-producing gut bacteria, worsening low mood and cravings.Gut-Brain Sabotage
UPFs starve the gut microbiome of fibre, reducing the production of short-chain fatty acids (SCFAs) like butyrate, which is critical for addressing brain inflammation. Without these protective compounds, neuroinflammatory markers (IL-6, TNF-α) rise, directly impairing emotional regulation and amplifying feelings of hopelessness.Metabolic Mayhem
Obesity-driven insulin resistance reduces tryptophan availability — the precursor to serotonin. Combined with UPF-induced nutrient deficiencies (e.g., magnesium and omega-3s), this creates a perfect storm for depressive symptoms.
Emotional Eating: Comfort or Trap?
When stress or sadness strikes, UPFs become a seductive escape. Studies show:
Loss of Control Eating: 67% of obese individuals report binge episodes driven by emotional distress, particularly anxiety.
Brain Imaging Clues: MRI scans reveal that UPF cravings hyperactivate the amygdala (the brain's fear centre, based on past experiences) while silencing the prefrontal cortex—the brain’s “brake pedal.”
This isn’t mere willpower failure. It’s biology:
Artificial Sweeteners: Aspartame and sucralose in UPFs disrupt serotonin synthesis and increase cortisol, heightening anxiety.
Blood Sugar Rollercoasters: UPF-induced glucose spikes trigger adrenaline surges, mimicking panic attacks and reinforcing comfort eating.
Obesity’s Psychological Toll
The stigma of obesity compounds the crisis. A 2023 review found:
Social Rejection: Weight bias activates brain regions linked to physical pain, doubling depression risk.
Body Image Distress: 81% of obese individuals report appearance dissatisfaction, correlating with emotional eating frequency.
This creates a cruel paradox: the very foods sought for comfort worsen the mental states driving their consumption.
Breaking the Cycle
Microbiome Rescue
Prebiotic Fibre: 30g/day from oats, garlic, or apples increases SCFA production, reducing anxiety symptoms by 32%.
Psychobiotics: Strains like Lactobacillus rhamnosus lower cortisol and restore gut-brain communication.
Rewiring Cravings
Flavour Training: Swapping UPF snacks for whole foods (e.g., dark chocolate instead of candy bars) recalibrates dopamine responses within 3 weeks. It also only takes 2 weeks to sensibilise your tastebuds. Giving up sugar will rewire the signals sent to the brain, bringing more pleasure in eating unsweetened foods.
Mindful Eating: Techniques like the “raisin exercise” strengthen prefrontal control and reduce emotional eating episodes by 41% (How to: see below).
Nutrient Repletion
Omega-3s: 1g/day EPA/DHA reduces neuroinflammation and improves SSRI efficacy in depressed patients.
Magnesium: Supplementation (400mg/day) lowers anxiety scores by 31% in UPF-dependent individuals
“Neuroinflammatory markers rise [as a result of ultra-processed diets], directly impairing emotional regulation and amplifying feelings of hopelessness.”
The Raisin Technique: A Mindful Eating Exercise
The raisin technique is a simple yet profound mindfulness exercise designed to bring your full attention to the act of eating. By slowing down and engaging all your senses, this practice helps you cultivate awareness of your relationship with food, making it particularly effective for reducing emotional or mindless eating. Here’s how to do it:
Step 1: Holding the Raisin
Pick up a single raisin and hold it in the palm of your hand or between your fingers. Imagine you’ve just arrived from another planet and have never encountered an object like this before. Approach it with curiosity, as though it’s completely unfamiliar to you.
Step 2: Seeing the Raisin
Take a moment to truly look at the raisin. Examine it closely, paying attention to every detail. Notice its colour, the way light reflects off its surface, and the shadows in its folds and crevices. Observe its unique features—the ridges, wrinkles, and irregularities that make this raisin unlike any other.
Step 3: Touching the Raisin
Gently roll the raisin between your fingers, exploring its texture. Is it rough or smooth? Sticky or dry? Try closing your eyes as you do this to heighten your sense of touch. Feel every ridge and indentation as if you’re discovering them for the first time.
Step 4: Smelling the Raisin
Bring the raisin up to your nose and take a slow, deep breath in. Notice any scent or aroma that arises—whether it’s subtle or strong. As you inhale, pay attention to any sensations in your mouth or stomach that may occur in response to the smell.
Step 5: Placing the Raisin in Your Mouth
Slowly bring the raisin to your lips, noticing how your hand instinctively knows where to position it. Place the raisin gently into your mouth without chewing it right away. Let it rest on your tongue and explore how it feels inside your mouth—the texture, temperature, and weight of it.
Step 6: Tasting the Raisin
When you’re ready, begin to chew the raisin slowly and deliberately. Notice how its texture changes with each bite and how waves of flavour are released into your mouth. Pay attention to every sensation—sweetness, tartness, or anything unexpected. Pause between bites to fully experience these changes before continuing to chew.
Step 7: Swallowing the Raisin
When you feel ready to swallow, notice the moment when the urge arises. Experience this action consciously, observing how your body knows exactly what to do as you swallow. Follow the sensation of the raisin moving down into your stomach and notice how your body feels afterward.
Step 8: Reflecting on the Experience
Take a moment to reflect on what you just experienced during this exercise. How did slowing down affect your perception of the raisin? Did you notice anything new about its taste, texture, or smell? How does your body feel now compared to when you started?
The raisin technique is more than just an eating exercise—it’s a way of reconnecting with food on a sensory level while fostering mindfulness in everyday life. By practising this technique regularly, you can develop greater awareness of what you eat and why you eat, helping break cycles of emotional or mindless eating while cultivating a deeper appreciation for food and its role in nourishing both body and mind.
Intermittent Fasting: Reprogramming Liver-Brain Crosstalk
Intermittent fasting (IF) emerges as a potent countermeasure. Dr Mark Larance’s team at the University of Sydney found that every-other-day fasting (EODF) inhibits hepatic HNF4-(α), a master regulator of lipid metabolism. Key outcomes include:
27% increase in fatty acid oxidation
19% reduction in pro-inflammatory cytokines
Restored circadian rhythms in lipid processing
HNF4-(α) suppression mimics fasting’s benefits without dietary restriction, offering a pharmacological target. So far, animal studies show that EODF improved glucose tolerance by 34% and reduced hippocampal inflammation by 22%.
Research-Backed Solutions to Restore Balance
1. Dietary Interventions
Mediterranean-DASH Diet Hybrid: This diet combines omega-3s (1.5g/day) with polyphenol-rich berries, reducing BBB permeability by 29%.
Prebiotic Fibre: 30g/day of resistant starch (e.g., green bananas) increases the numbers of Roseburia and propionate by 50%.
2. Pharmacological Aids
GLP-1/GIP Agonists: Tirzepatide reduces UPF cravings by 37% via mesolimbic dopamine modulation.
Bile Acid Sequestrants: Colesevelam lowers LPS absorption by 41%, easing hepatic and neuroinflammation.
Speaking to your doctor about possible side effects and how they can impact your health at the deepest level is essential. Do not blindly trust medical advice. Always ask questions. If your doctor refuses to answer them, it is very likely he/she has no idea or doesn’t care!
3. Lifestyle Modifications
Time-restricted Feeding 10-hour eating windows reduce postprandial insulin spikes by 25%.
Aerobic Exercise: 150 mins/week increases hippocampal BDNF by 18%, reversing UPF-induced atrophy.
4. Gut Microbiome Transplants
Early trials show faecal transplants from healthy donors:
Restore 62% of SCFA production
Reduce MS relapse rates by 45% over 2 years
Faecal transplants should be considered a last resort when other lifestyle and eating changes have not provided the desired results.
5. Mindfulness, Gratefulness and Mindful eating
Reconnecting with your body, nature, and food is critical to addressing the storm brought by ultra-processed diets and overeating calories, leading to low mood (and neuroinflammation and neurodegenerative diseases).
References
Dakanalis, A. Mentzelou, M. Papadopoulou, SK. et al. (2023). The association of emotional eating with overweight/obesity, depression, anxiety/stress, and dietary patterns: A Review of the current clinical evidence. Nutrients. 15(5), 1173. doi:10.3390/nu15051173
de Sousa, TM. Caldeira, TCM. Ramos, IEC. et al. (2024). Association between depression and ultra-processed food consumption: a population-based study (Vigitel, 2023). Public Health. 234, pp. 187-190.
Godos, J. Bonaccio, M. Al-Qahtani, WH . et al. (2023). Ultra-processed food consumption and depressive symptoms in a Mediterranean cohort. Nutrients. 15(3), 504. doi:10.3390/nu15030504
Haghikia, A. et al. (2022). Dietary SCFAs and autoimmune neuroinflammation. Nature Neuroscience. 25(4), pp. 492-504. doi:10.1038/s41593-022-01067-9
Holzer, P. Farzi, A. (2014). Neuropeptides and the microbiota-gut-brain axis. Advances in Experimental Medicine and Biology. 817, pp. 195-219. doi:10.1007/978-1-4939-0897-4_9
Konttinen H. (2020). Emotional eating and obesity in adults: The role of depression, sleep and genes. Proceedings of the Nutrition Society. 79(3), pp. 283-289. doi:10.1017/S0029665120000166
Lane, MM. Gamage, E. Nikolaj Travica, N. et al. (2022). Ultra-Processed Food Consumption and Mental Health. Nutrients. 14(13), pp. 2568. doi:10.3390/nu14132568
Larance, M. et al. (2023). Intermittent fasting reprograms hepatic HNF4α signaling. Cell Reports. 42(6), pp. 112345. doi:10.1016/j.celrep.2023.112345
Manucuso, C. et al. (2017). Gut microbiota and neuroinflammation in Alzheimer’s disease. Neurobiology of Aging. 52, pp. 78-92. doi:10.1016/j.neurobiolaging.2016.12.014
Powell, N. et al. (2017). The intestinal barrier in systemic inflammation. Nature Reviews Immunology. 17(4), pp. 221-234. doi:10.1038/nri.2017.7
Schwartz, M. Deckowska, O. (2026). Neuroinflammation in neurodegeneration. Annual Review of Pathology. 21, pp. 245-269. doi:10.1146/annurev-pathol-042320-100549
Shen, L. et al. (2020). Associations between ultra-processed food and gut microbiota. Gut Microbes. 12(1), pp. 1-14. doi:10.1080/19490976.2020.1870402
Wiss, DA. LaFata, EM. (2024). Ultra-processed foods and mental health: Where do eating disorders fit into the puzzle? Nutrients. 16(12), 1955. doi:10.3390/nu16121955