Obesity Begins in the Brain: Is there more to the Gut-Brain Axis?
The global obesity crisis is reaching alarming proportions, with projections indicating that by 2035, 1.9 billion people worldwide will be living with obesity. This epidemic not only poses significant health risks but also places an enormous economic burden on healthcare systems and economies, with an estimated annual cost of £4.32 trillion.
For decades, obesity has been viewed primarily through the lens of energy balance – calories in versus calories out. However, recent neuroscientific research is challenging this simplistic perspective, revealing that obesity is not merely a metabolic disorder but a complex brain-driven phenomenon.
The Brain’s Role in Obesity
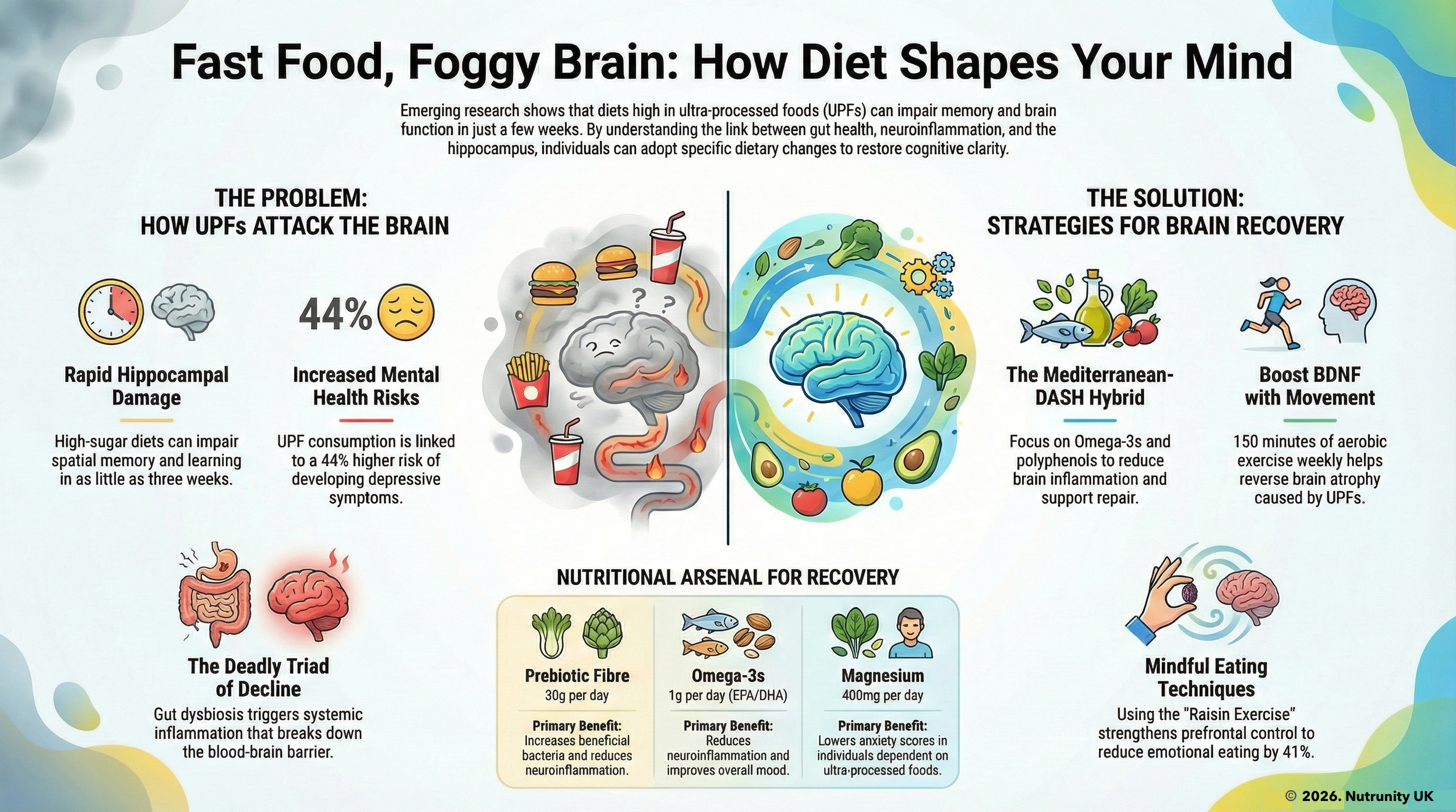
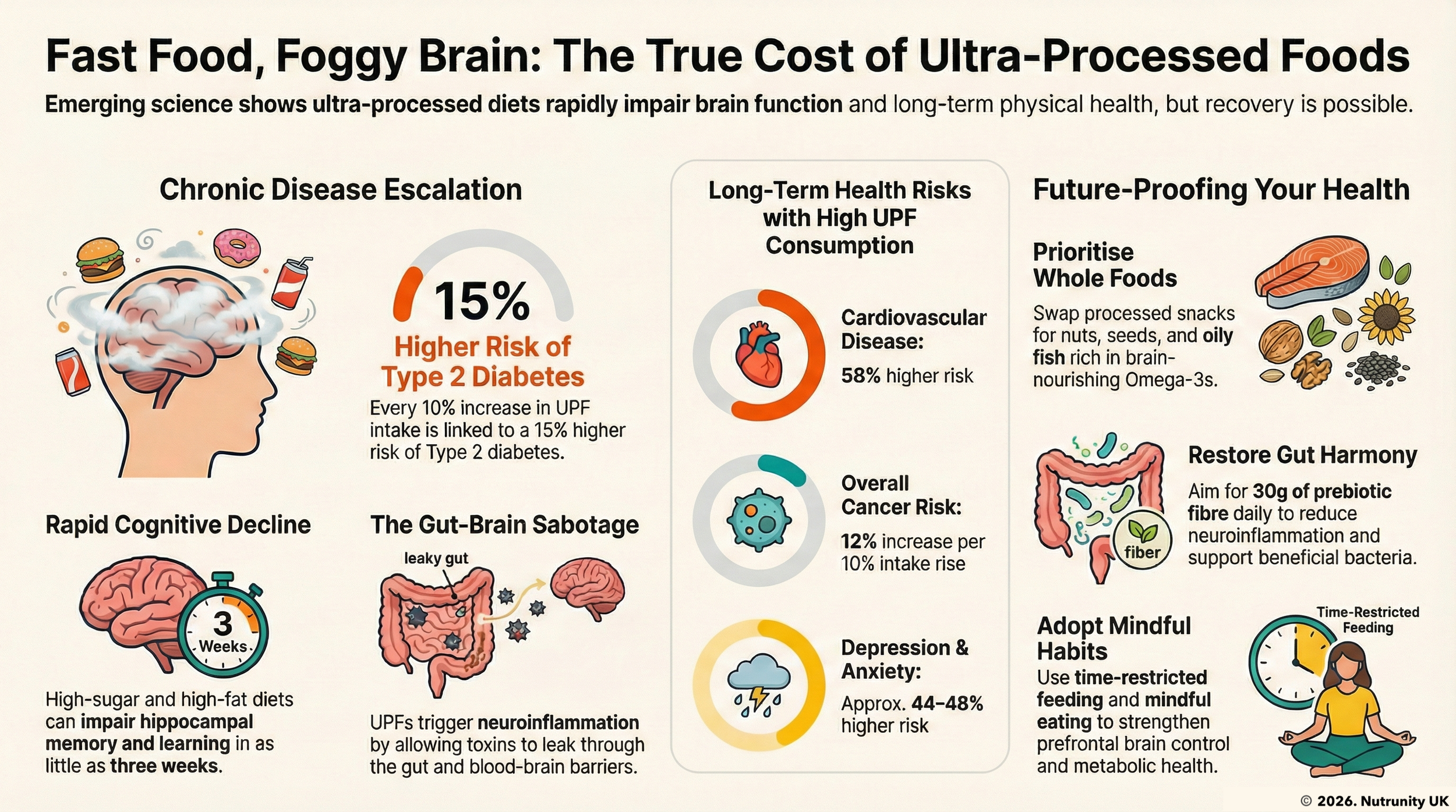
Emerging evidence suggests that the brain’s response to food and metabolic signals may be the critical missing link in understanding obesity and its long-term impact. Recent studies have shown that even short-term overconsumption of ultra-processed foods can disrupt brain function and alter metabolic processes, even before visible weight gain occurs.
Neurological Changes Precede Weight Gain
A groundbreaking study from the University of Tübingen has revealed that a brief period of overeating high-calorie, ultra-processed foods can significantly alter brain insulin responsiveness and trigger liver fat accumulation — all before any detectable weight gain. This research challenges conventional understanding, suggesting that the brain undergoes metabolic changes long before the body shows signs of obesity.
“Even short-term overconsumption of ultra-processed foods can disrupt brain function and alter metabolic processes, even before visible weight gain occurs.”
The small study had 29 healthy-weight participants and found that after just five days of high-calorie intake:
Participants exhibited heightened insulin activity in brain regions that were responsible for food reward and decision-making.
Liver fat accumulation increased significantly, directly correlating with altered brain response to insulin.
One week after resuming a normal diet, participants showed a decline in brain insulin activity in key regions such as the hippocampus and fusiform gyrus.
Reward learning was impaired, with participants becoming less sensitive to rewards and more sensitive to punishments.
White matter integrity between reward and cognitive brain regions was reduced.
These findings suggest that even short-term exposure to unhealthy diets can cause lasting neurological and metabolic changes that persist beyond the period of indulgence.
Brain Insulin Resistance
New findings highlight how systemic inflammation and oxidative stress, common in obesity, can disrupt the blood-brain barrier, leading to brain insulin resistance. This disruption is linked to impaired cognitive function and metabolic regulation, providing a clearer picture of how obesity affects the brain.
Obesity-induced mitochondrial changes, such as increased reactive oxygen species production and reduced ATP content, suggest that mitochondrial health is critical for maintaining proper insulin signalling in the brain.
Dysregulation of the gut-brain axis, influenced by unhealthy diets, can contribute to obesity by altering appetite regulation, glucose metabolism, and even mood and cognition.
Research demonstrates that individuals with high brain insulin sensitivity achieve greater weight loss during lifestyle interventions and are less likely to regain weight over time. This highlights the predictive value of brain insulin responsiveness in long-term obesity management.
Obesity-related brain insulin resistance is linked to memory, learning, and executive function deficits. These cognitive impairments may result from neuroinflammation and disrupted signalling within the gut-brain axis, further bringing attention to the neurological consequences of obesity
it is important to indicate that chronic stress, anxiety disorders and depression impact gut health, brain health and mood at the deepest levels, contributing to faster onset and worse outcomes than just insulin dysregulation due to a bad diet. These conditions are often implicated in insulin dysfunction, obesity and poor cognition.
Rethinking Obesity as a Neurological Condition
Traditionally, obesity has been associated with peripheral insulin resistance. However, this new research suggests that brain insulin resistance may precede metabolic dysfunction and weight gain, making it a critical early marker for obesity risk.
Key Implications:
Brain-Driven Condition:
Obesity isn’t just about body fat; it’s also a brain-driven condition where short-term dietary choices can cause lasting disruptions in brain insulin signalling.
Altered Reward Pathways:
Overeating ultra-processed foods alters brain reward pathways, potentially explaining why unhealthy eating habits persist.
Early Warning Signs:
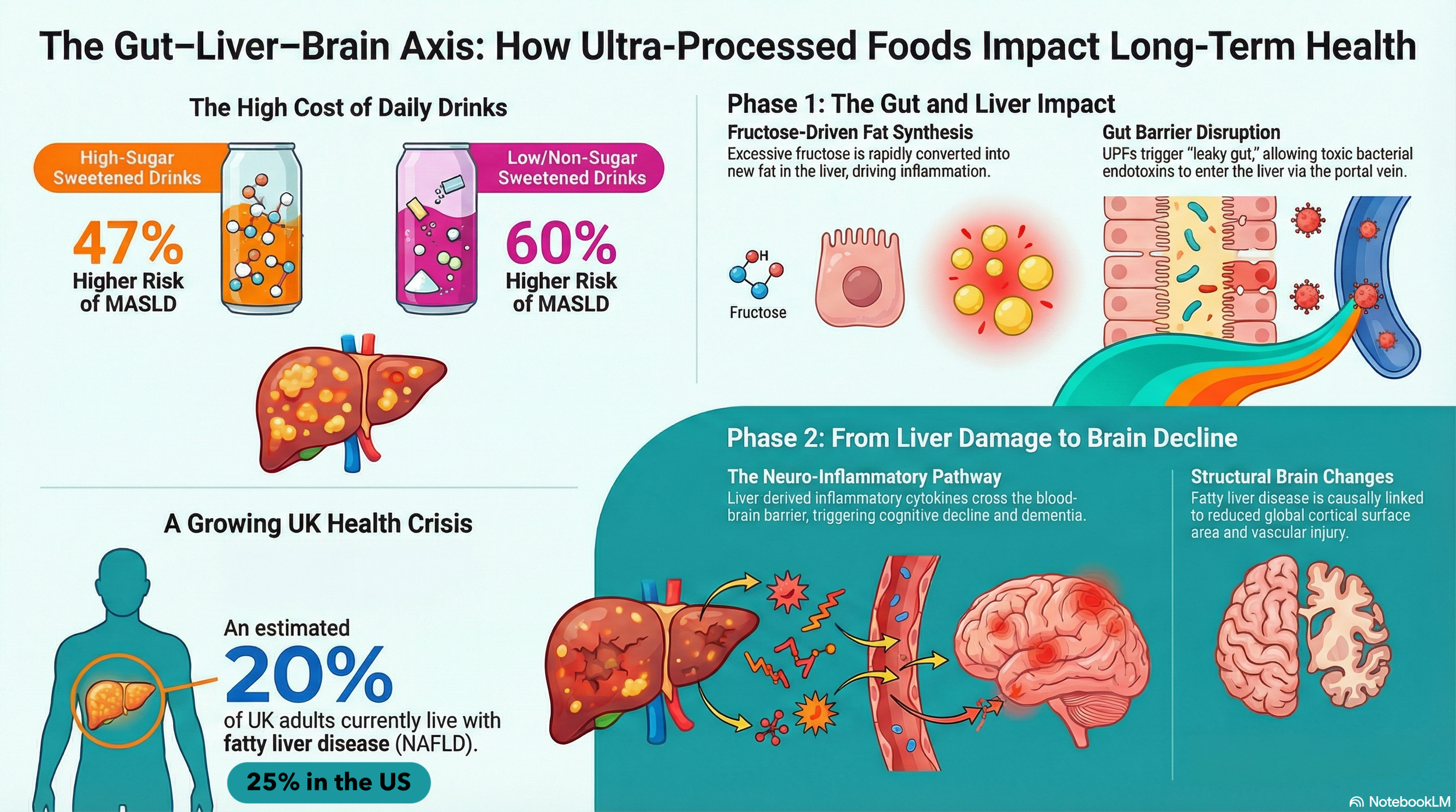
Liver fat accumulation is an early warning sign, indicating internal metabolic shifts long before visible weight changes. Non-alcoholic fatty liver disease (NAFLD) is also a consequence of gut dysfunction and dysbiosis (some pathogenic bacteria produce alcohol and pro-inflammatory substances that inflame the liver).
Long-Term Consequences:
Impaired reward learning persisted after participants resumed a normal diet, indicating long-term consequences of short-term indulgence.
The Gut-Brain Axis in Obesity
The research also highlighted the importance of the gut-brain axis in obesity. This complex bidirectional communication system, mediated by hormonal, immunological, and neural signals, is crucial in energy homeostasis and cognitive function.
Key Findings:
Dysregulation of the gut-brain axis communication is associated with metabolic diseases and psychiatric disorders.
Alterations in gut microbiota composition or function can disrupt the molecular dialogue between the gut and brain, mood and cognition.
Western dietary patterns (e.g., the SAD diet), which are rich in simple sugars and trans fat (while providing little to no dietary prebiotic fibre), reduce microbial diversity, promote inflammation, and contribute to increased intestinal permeability.
The role of ultra-processed diet on gut microbiota, gut-brain axis and cognitive function compared to the role of a nutrient-dense diet on health and mental health.
Implications for Prevention and Treatment
If obesity starts in the brain, our prevention and treatment strategies should begin there, too. To effectively address obesity, brain health must be prioritised in weight management strategies, recognising that both cognitive and metabolic changes play a crucial role in obesity development.
Strategies:
Brain-Focused Interventions:
Preventive programmes should consider how the brain regulates hunger, reward responses, and insulin signalling alongside traditional metabolic factors.
Reducing Ultra-Processed Food Intake:
Even short-term reductions in ultra-processed food consumption may be essential to prevent lasting effects on brain function and metabolic health.
Targeting Brain Insulin Resistance:
Future obesity interventions must restore brain insulin sensitivity before weight gain begins.
Gut Microbiota Modulation:
Dietary strategies promoting a healthy gut microbiota (e.g., probiotics, fibre-rich diets) could beneficially impact obesity and its mental complications.
While these findings provide valuable insights, more long-term research is needed to fully understand the relationship between brain insulin action, dietary choices, and obesity progression. As science continues to evolve, understanding how the brain processes food, rewards, and metabolic signals could be missing in combating the global obesity epidemic.
By recognising obesity as a brain-driven condition, we open new avenues for prevention and treatment that go beyond simple calorie counting. This paradigm shift could lead to more effective, personalised approaches to weight management and ultimately help curb the rising tide of obesity worldwide.
References
Agustí, A. García-Pardo, MP. López-Almela, I. et al. (2018). Interplay between the gut-brain axis, obesity and cognitive function. Frontiers in Neuroscience. 12:155. doi:10.3389/fnins.2018.00155
Apryatin, SA. Sidorova, YS. Shipelin, V.A. et al. (2017). Neuromotor activity, anxiety and cognitive function in the in vivo model of alimentary hyperlipidemia and obesity. Bulletin of Experimental Biology and Medicine. 163, pp. 37–41. doi:10.1007/s10517-017-3732-z
Asadi, A. Shadab Mehr, N. Mohamadi, MH. et al. (2022). Obesity and gut-microbiota-brain axis: A narrative review. Journal of Clinical Laboratory Analysis. 36(5), e24420. doi:10.1002/jcla.24420
Beilharz, JE. Maniam, J. and Morris, MJ. (2015). Diet-induced cognitive deficits: The role of fat and sugar, potential mechanisms and nutritional interventions. Nutrients 7, pp. 6719–6738. doi:10.3390/nu7085307
Brierley, SM. Linden, DR. (2014). Neuroplasticity and dysfunction after gastrointestinal inflammation. Nature Reviews Gastroenterology & Hepatology. 11, pp. 611–627. doi:10.1038/nrgastro.2014.103
Brinkworth, GD. Buckley, JD. Noakes, M. et al. (2009). Long-term effects of a very low-carbohydrate diet and a low-fat diet on mood and cognitive function. Archives of Internal Medicines. 169, pp. 1873–1880. doi:10.1001/archinternmed.2009.329
Bruce-Keller, AJ. Salbaum, J.M. Luo, M. et al. (2015). Obese-type gut microbiota induce neurobehavioral changes in the absence of obesity. Biological Psychiatry. 77, pp. 607–615. doi:10.1016/j.biopsych.2014.07.012
Carabotti, M. Scirocco, A. Maselli, M. A. et al. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals in Gastroenterology. 28, pp. 203–209.
Castanon, N. Lasselin, J. Capuron, L. (2014). Neuropsychiatric comorbidity in obesity: role of inflammatory processes. Frontiers in Endocrinology. 5:74. doi:10.3389/fendo.2014.00074
Cenit, MC. Sanz, Y. Codoner-Franch, P. (2017). Influence of gut microbiota on neuropsychiatric disorders. World Journal of Gastroenterology. 23, pp. 5486–5498. doi:10.3748/wjg.v23.i30.5486
Cheke, LG. Simons, JS. Clayton, NS. (2016). Higher body mass index is associated with episodic memory deficits in young adults. Quarterly Journal of Experimental Psychology. 69, pp. 2305–2316. doi:10.1080/17470218.2015.1099163
Collison, KS. Makhoul, NJ. Inglis, A. et al. (2010). Dietary trans-fat combined with monosodium glutamate induces dyslipidemia and impairs spatial memory. Physiology and Behaviour. 99, pp. 334–342. doi:10.1016/j.physbeh.2009.11.010
Cryan, JF. O'Mahony, SM. (2011). The microbiome-gut-brain axis: from bowel to behavior. Neurogastroenterology and Motility. 23, pp. 187–192. doi:10.1111/j.1365-2982.2010.01664.x
de Wit, L. Luppino, F. van Straten, A. et al. (2010). Depression and obesity: A meta-analysis of community-based studies. Psychiatry Research. 178, pp. 230–235. doi:10.1016/j.psychres.2009.04.015
Grenham, S. Clarke, G. Cryan, JF. et al. (2011). Brain-gut-microbe communication in health and disease. Frontiers in Physiology. 2, 94. doi:10.3389/fphys.2011.00094
Gupta, A. Osadchiy, V. Mayer, EA. (2020). Brain–gut–microbiome interactions in obesity and food addiction. Nature Reviews Gastroenterology & Hepatology. 17, pp. 655–672. doi:10.1038/s41575-020-0341-5
Heni, M. (2024). The insulin resistant brain: Impact on whole-body metabolism and body fat distribution. Diabetologia. 67(7), pp. 1181-1191. doi:10.1007/s00125-024-06104-9
Hyland, NP. Cryan, JF. (2016). Microbe-host interactions: Influence of the gut microbiota on the enteric nervous system. Developmental Biology. 417, pp. 182–187. doi:10.1016/j.ydbio.2016.06.027
Kreier, F. Kap, YS. Mettenleiter, TC. et al. (2006). Tracing from fat tissue, liver, and pancreas: A neuroanatomical framework for the role of the brain in type 2 diabetes, Endocrinology. 147(3), pp. 1140–1147, doi:10.1210/en.2005-0667
Kullmann, S. Goj, T. Veit, R. et al. (2022). Exercise restores brain insulin sensitivity in sedentary adults who are overweight and obese. JCI Insight. 7(18), e161498. doi:10.1172/jci.insight.161498
Kullmann, S. Valenta, V. Wagner, R. et al. (2020). Brain insulin sensitivity is linked to adiposity and body fat distribution. Nature Communications. 11, 1841. doi:10.1038/s41467-020-15686-y
Sripetchwandee, J. Chattipakorn, N. Chattipakorn, SC. (2018). Links between obesity-induced brain insulin resistance, brain mitochondrial dysfunction, and dementia. Frontiers in Endocrinology. 9:496. doi:10.3389/fendo.2018.00496