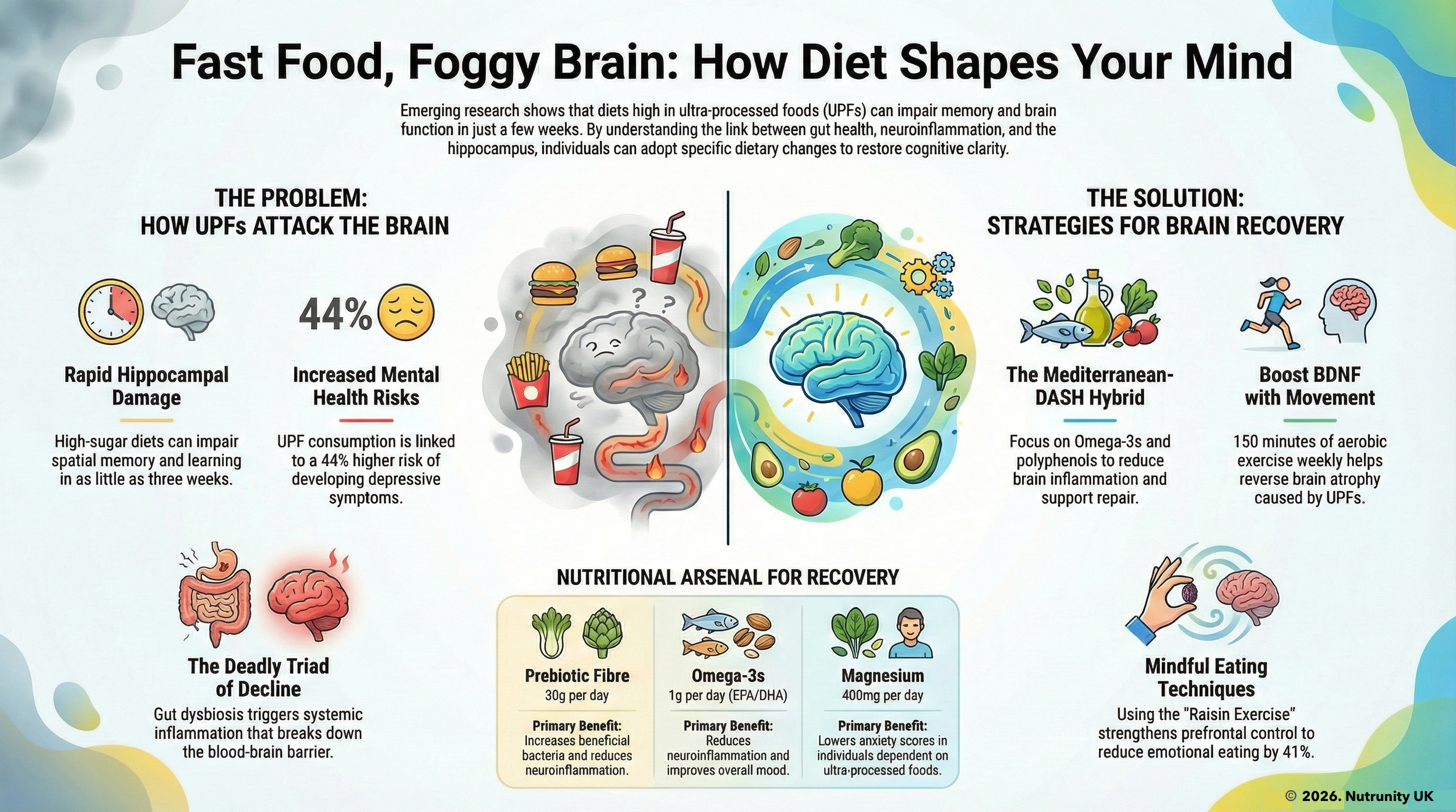
Fast Food, Foggy Brain: How High Sugar and High Fat Diets Impact Cognition
Fast food and sugary drinks are everywhere — quick, cheap, and tempting. But emerging science is revealing a sobering truth: diets high in fat and sugar can impair memory and cognitive function in a matter of weeks, even in young, healthy individuals.
While the link between junk food, weight gain, and metabolic dysregulation is well known, research shows that poor dietary choices may negatively impact essential brain function.
The Surprising Link Between Diet and Brain Function
For decades, the dangers of fast food were thought to be limited to weight gain and metabolic issues. However, a landmark study from the University of Sydney, published in the International Journal of Obesity, has shown that diets high in saturated fat and sugar, especially those rich in fast food and sugary drinks, can impair brain function in as little as a few weeks. The research involved healthy adults aged 18–38, tested on their ability to recall the location of hidden objects in a virtual maze, a measure of spatial memory governed by the hippocampus.
The results were striking: those with higher intakes of ultra-processed foods performed significantly worse on memory tasks, regardless of their body weight or fitness level.
This finding is echoed by additional studies showing that the modern Western diet, rich in trans fats, refined sugars, and ultra-processed ingredients, triggers inflammation and oxidative stress in the brain, leading to memory issues, mood changes, and even early cognitive decline.
Interestingly, these cognitive changes appeared before any outward signs of poor health, such as weight gain or metabolic issues. This means that even if you feel fit and look healthy, a diet high in trans/saturated fat and sugar can quietly erode your brain’s performance.
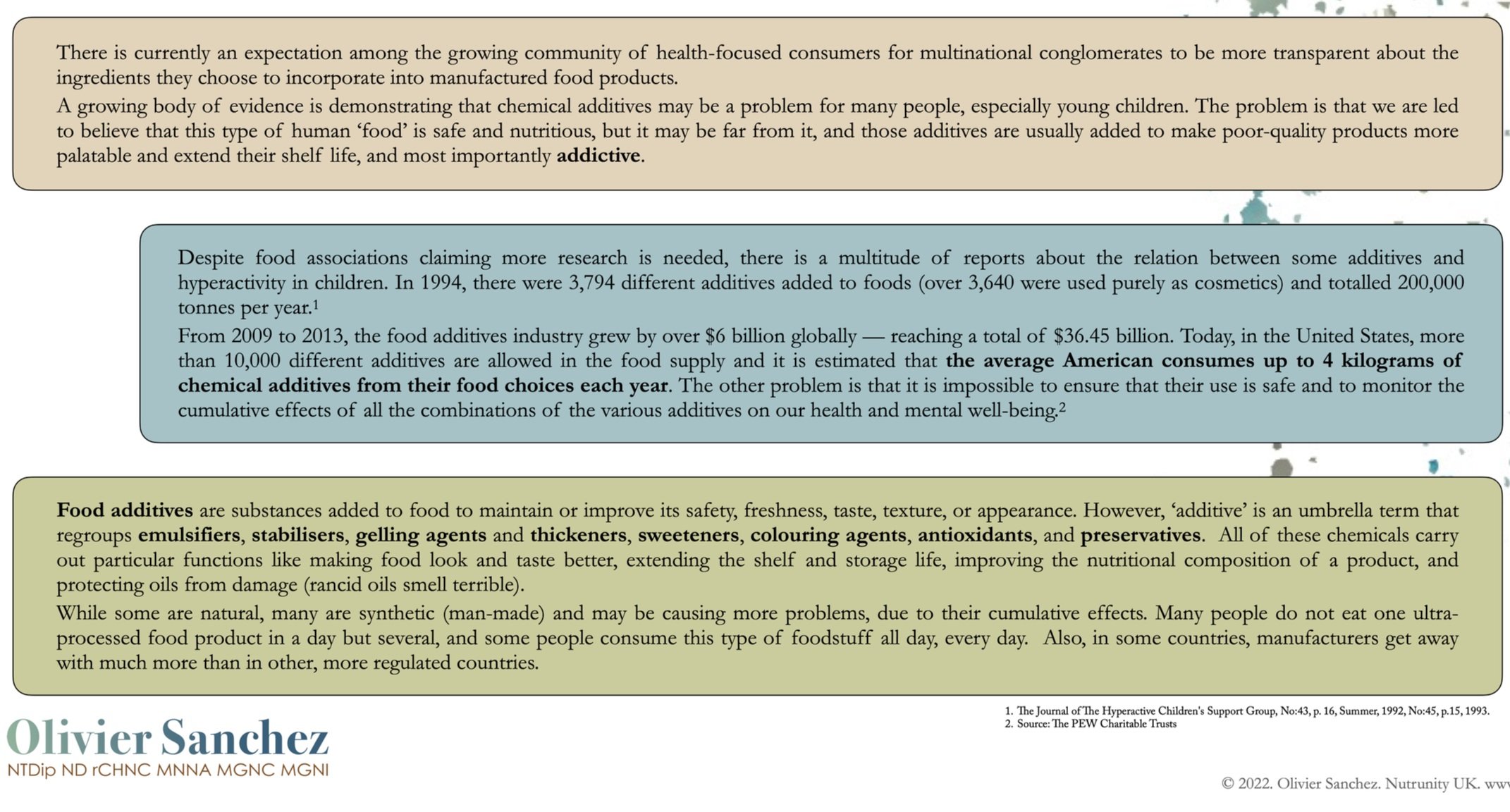
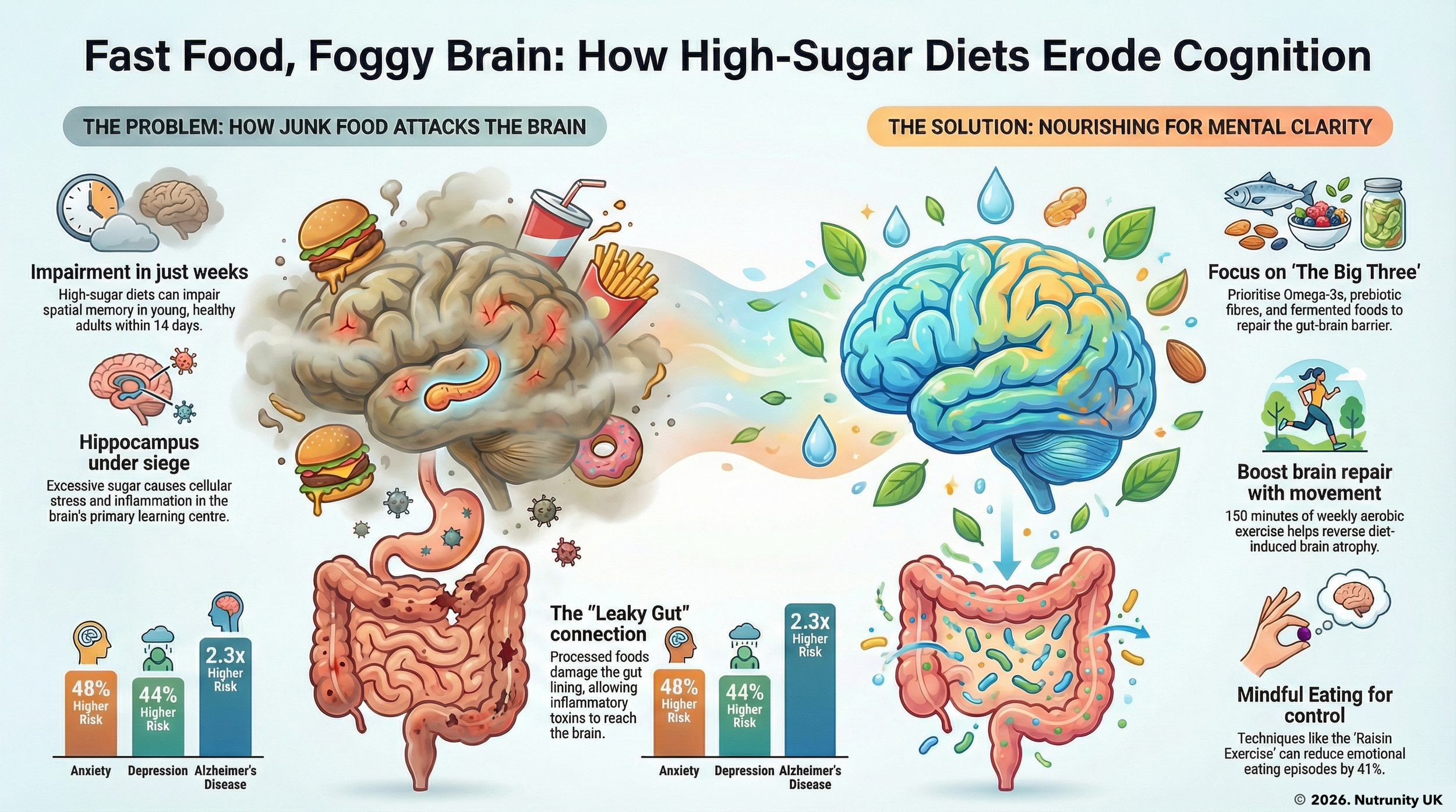
The impact of UPFs on health - how synthetic additives and other chemicals in the food we eat affect us
This is what the Texas Institute for Neurological Disorders responded:
“Excessive sugar consumption can lead to memory deficiencies, sugar addiction, and overall health deficiencies.
The American Heart Association recommends no more than 25 grams of added sugar per day for women and 38 grams for men. However, most Americans consume much more than the recommended amount of sugar per day. The best way to reduce the consumption of foods high in sugars is by eating a natural diet consisting of real foods.
The brain uses energy in the form of glucose to fuel cellular activities. However, a high sugar diet can lead to excess glucose in the brain and studies have linked excess glucose consumption to memory and cognitive deficiencies. Another reason sugar is harmful to the brain is because it affects certain neurotransmitters, which can result in sugar addictions.
Dopamine is a neurotransmitter in the brain and some of the processes it controls include: mood, behavior, learning, and memory. Drug addiction and Parkinson’s disease are some examples of conditions associated with disrupted dopamine levels. Sugar can also disrupt dopamine levels as the brain becomes used to high levels of sugar. In fact, both the gene expression and availability of dopamine receptors can be altered in certain areas of the brain from consuming too much sugar over a long period of time. The effect sugar has on dopamine and dopamine receptors make it addictive and is why it is often so difficult to eliminate sugar from the diet.
Not only is sugar harmful to the health of the brain, but it is also harmful to the overall health of the body. Too much sugar can lead to tooth decay and cavities, leading to oral health problems. In addition, excessive sugar can lead to weight gain and increases the risk of developing Type 2 Diabetes. Insulin is a hormone that helps to metabolize sugar in the body, but if there is too much sugar in the body then insulin resistance can occur. Eventually, insulin resistance may lead to Type 2 Diabetes.
Excessive sugar consumption is harmful to brain health, and can lead to memory deficiencies, sugar addiction, and decline in overall health. To keep your brain healthy, consume sugar in moderation and within the recommended guidelines.”
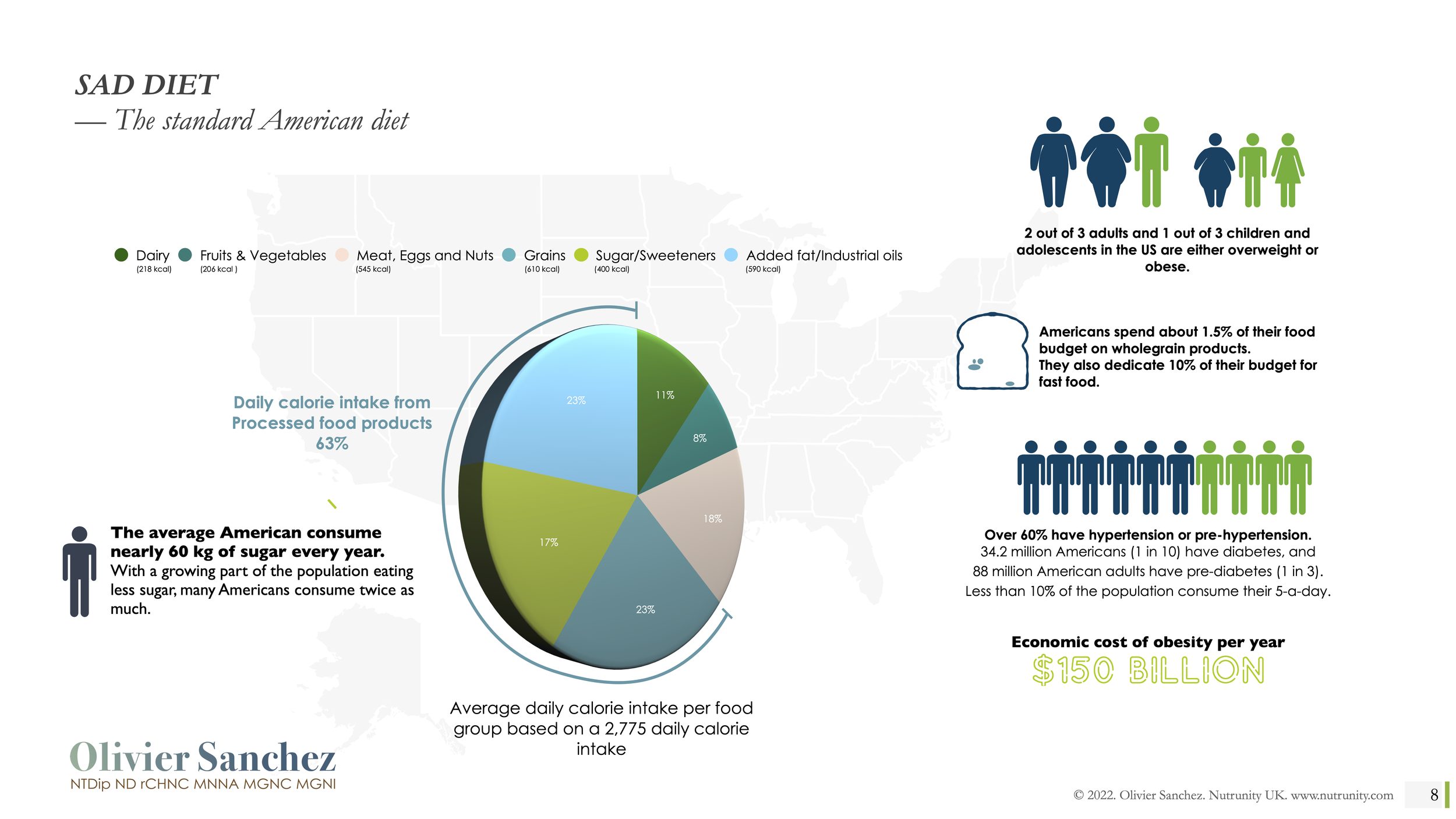
The SAD diet, food intake and health consequences
How Sugar and Fat Target the Hippocampus
The hippocampus is at the heart of these discoveries, a seahorse-shaped region crucial for memory, learning, and spatial navigation. It is not just responsible for remembering passwords or where you parked your car. It is central to learning, spatial navigation, and processing new experiences. This small, seahorse-shaped region is especially vulnerable to dietary insults, and poor nutrition can quickly undermine its function.
In the University of Sydney study, participants who ate more fries, pizza, sweets, and soft drinks performed worse on spatial memory tasks, even if they were young and physically fit.
Why is the hippocampus so sensitive to what you eat?
Cellular Stress: Diets rich in sugar and trans/saturated fat increase the production of reactive oxygen species (ROS), damaging neurones and other brain cells.
Inflammatory Responses: High-fat, high-sugar diets activate immune cells in the brain, leading to chronic inflammation that disrupts memory and learning.
Disrupted Metabolic Signalling: The hippocampus depends on a delicate balance of neurotransmitters and energy molecules. Poor nutrition throws this system off, reducing brain plasticity and efficiency.
Studies show these effects can manifest in just a few weeks. Cognitive impairments, such as trouble concentrating, forgetfulness, and difficulty navigating new environments, can develop even in young, active adults.
Beyond Memory: The Broader Impact of UPF Diets
The dangers of high-fat, high-sugar diets go beyond memory lapses. Research links these eating patterns to a cascade of adverse effects, including:
Mood Disorders: Diet-driven neuroinflammation and gut dysbiosis are linked to higher rates of depression and anxiety.
Neurodegenerative Disease Risk: Chronic consumption of ultra-processed foods (UPFs) increases the risk of Alzheimer’s disease by more than twofold, primarily due to persistent inflammation and blood-brain barrier breakdown.
Emotional Eating and Cravings: UPFs hijack the brain’s reward circuits, making it harder to regulate cravings and leading to a cycle of emotional eating and further cognitive decline.
The Gut-Brain Connection
The gut and brain are in constant communication. Diets high in sugar and fat disrupt the fragile gut ecosystem, reducing beneficial bacteria and short-chain fatty acids (SCFAs) that protect the gut lining and the brain. This gut dysbiosis allows inflammatory molecules to leak into the bloodstream (intestinal hyperpermeability), cross the blood-brain barrier, and impair cognitive function.
The connection between diet and cognition doesn’t stop at the brain. The gut microbiome plays a key role in brain health. Gut dysbiosis promotes the release and circulation of lipopolysaccharides (LPS), inflaming the liver and the brain. It also leads ti a decrease in SCFA production, which are critical for maintaining the gut lining and blood-brain barrier (BBB) integrity and suppressing neuroinflammation.
LPS and other inflammatory molecules flood the bloodstream when the gut barrier is compromised, triggering hepatic and systemic inflammation. This inflammatory cocktail degrades tight junctions in the BBB, allowing immune cells and cytokines to infiltrate the brain and further impair hippocampal function.
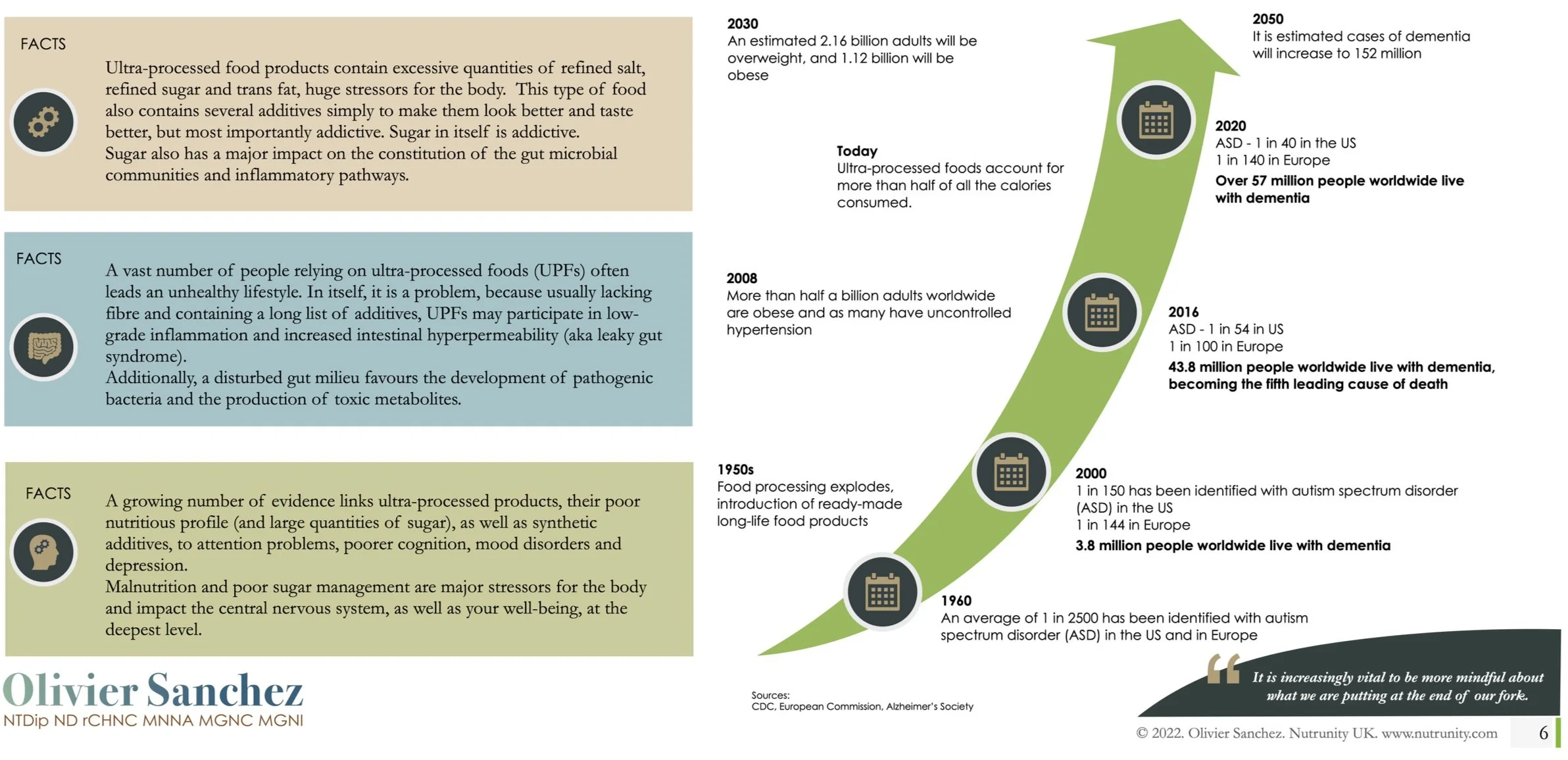
The impact of UPFs and their implications in metabolic disorders, mental ill-health and neurodegeneration
Fast Food, Mood, and Mental Health
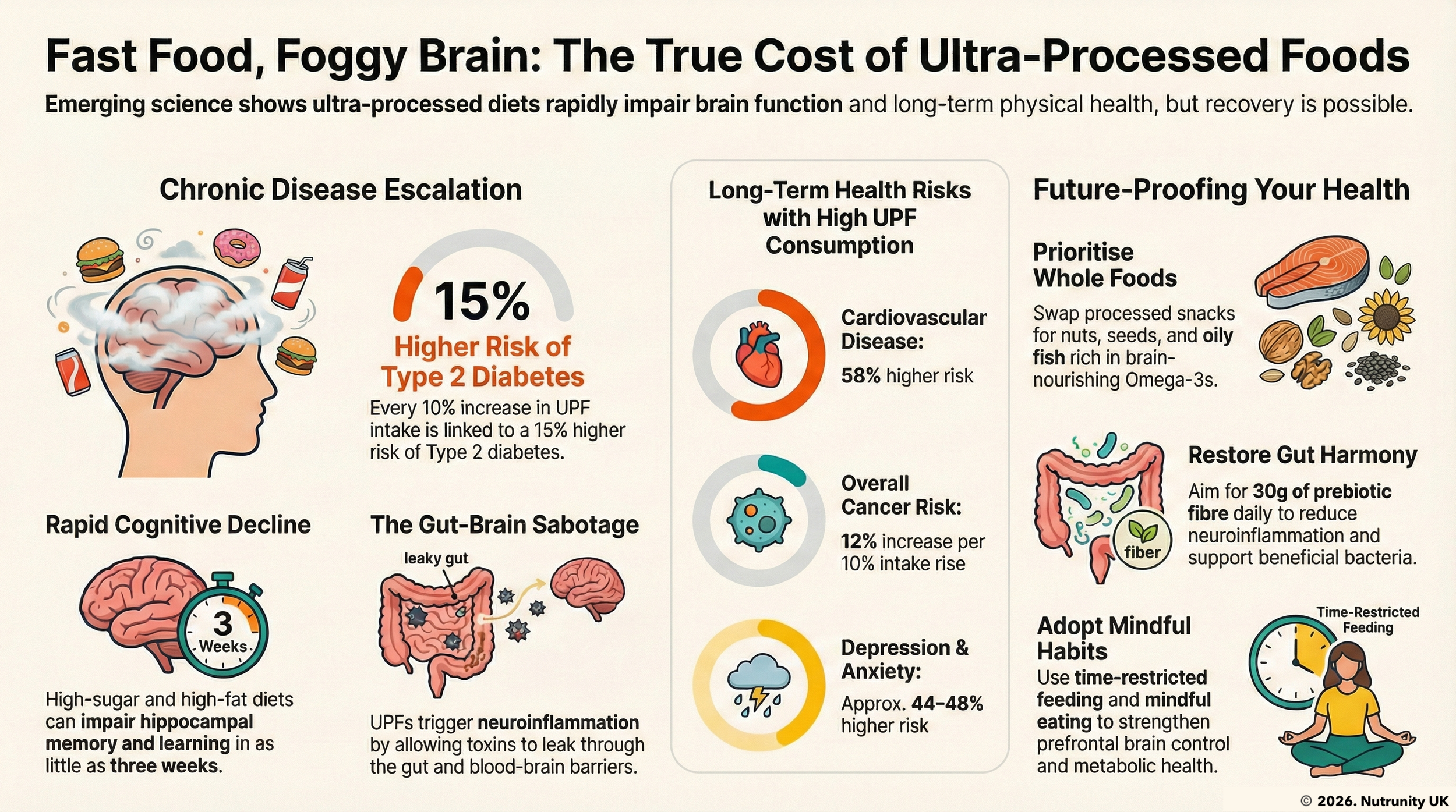
The impact of fast food and sugary diets extends beyond memory. High UPF consumption has been linked to a 44% higher risk of depression and a 48% higher risk of anxiety, according to a 2022 meta-analysis of over 385,000 individuals. This happens via three main pathways:
Neurochemical Hijacking: UPFs flood the brain with dopamine, creating short-lived euphoria but blunting natural reward circuits over time. This leads to cravings and emotional eating.
Gut-Brain Sabotage: UPFs starve the gut microbiome of fibre, reducing SCFA production and allowing neuroinflammatory markers (like IL-6 and TNF-α) to rise, which impairs emotional regulation. It also damages the balance between GABA and glutamate, making it difficult to maintain inflammatory defences and emotional balance.
Metabolic Mayhem: Metabolic dysfunction and obesity-driven insulin resistance reduces levels of tryptophan (the precursor to serotonin) in the brain. Combined with nutrient deficiencies (e.g., magnesium, omega-3s), this creates a storm for depressive symptoms.
MRI studies show that UPF cravings hyperactivate the amygdala (the brain’s fear centre) while silencing the prefrontal cortex, making it harder to control impulses and regulate emotions.
From Gut Dysbiosis to Neurodegeneration
The convergence of metabolic dysfunction, gut dysbiosis, and neuroinflammation forms a deadly triad that accelerates neurodegenerative diseases like Alzheimer’s and multiple sclerosis (MS). UPFs disrupt gut microbiota, provoke low-grade inflammation, and increase intestinal permeability, allowing LPS to flood the circulation and trigger hepatic inflammation. This not only contributes to non-alcoholic fatty liver disease (NAFLD) but also plays a key role in systemic and brain inflammation, leading to poorer cognition, pain in the joints and muscle stiffness.
Human studies confirm that UPF-heavy diets correlate with a 2.3x higher risk of Alzheimer’s, driven by chronic neuroinflammation and BBB leakage. In MS, UPFs deplete SCFA-producing bacteria, severely affecting propionic acid levels and impairing regulatory T-cell function, which worsens demyelination and neuroinflammation.
Emotional Eating: Comfort or a Trap?
Stress and sadness often drive people to seek comfort in high-calorie foods and drinks, but this is a trap. Studies show that 67% of obese individuals report binge episodes driven by emotional distress, particularly anxiety. Artificial sweeteners such as aspartame and sucralose disrupt serotonin synthesis and increase cortisol, another key player in anxiety disorders. UPF-induced glucose spikes cause adrenaline surges, mimicking panic attacks, which also lead to comfort eating.
Can the Brain Recover?
The good news is that the brain is resilient. Studies show that switching to a diet rich in whole foods, fibre, healthy fats (e.g., omega-3s), and antioxidants can restore hippocampal health and improve memory, even after periods of poor eating. A nutrient-dense diet, low in sugar, also promotes brain health by providing the building blocks for healing and repair processes. It is also essential to concentrate on regulating sleep, as the brain can only dispose of metabolic waste and toxins during deep sleep.
Research-Backed Solutions:
1. Dietary Interventions
Mediterranean-DASH Diet Hybrid: Combining omega-3s and polyphenol-rich berries reduces BBB permeability and supports brain health.
Prebiotic Fibre: 30g/day of resistant starch (e.g., green bananas, oats) increases beneficial gut bacteria and SCFA production, reducing anxiety and inflammation.
Key brain-nourishing choices include:
Fresh vegetables and fruits: Packed with antioxidants and fibre to reduce oxidative stress and support gut health.
Whole grains: Provide steady energy for optimal brain function.
Healthy oils: Olive, flaxseed, and avocado oils are rich in anti-inflammatory omega-3s and polyphenols.
Nuts and seeds: Offer vitamin E, magnesium, and healthy fats that protect neurons.
Fermented foods: Support a healthy microbiome and SCFA production.
2. Lifestyle Modifications
Intermittent Fasting: Every-other-day fasting increases fatty acid oxidation, reduces pro-inflammatory cytokines, and restores circadian rhythms in lipid processing.
Time-Restricted Feeding: 10-hour eating windows reduce postprandial insulin spikes and support metabolic health.
Aerobic Exercise: 150 minutes per week increases hippocampal BDNF, reversing UPF-induced brain atrophy.
3. Mindfulness and Mindful Eating
Techniques like the “raisin exercise” help you reconnect with food, slow down, and reduce emotional or mindless eating. Mindful eating has been shown to strengthen prefrontal control and reduce emotional eating episodes by 41%.
4. Nutrient Repletion
Omega-3s: 1g/day EPA/DHA reduces neuroinflammation and may improve mood.
Magnesium: 400mg/day lowers anxiety scores in UPF-dependent individuals
Lifestyle habits like regular exercise, quality sleep, and mindfulness enhance brain recovery and resilience.
Practical Steps to Protect Your Brain
1. Swap Processed Snacks for Whole Foods:
Choose fruit, nuts, or yoghurt over crisps, sweets, or pastries. Better yet, make your own delicious snacks. This way, you know exactly what goes in the recipe and can be in control of the sugar and fat content. Plus, it will help you reconnect with food, the key to optimum health and mental well-being.
2. Prioritise Omega-3s:
Eat oily fish (like sockeye salmon, mackerel, anchovies, sardines, herrings, and river trout) or plant-based sources (chia, flaxseed) several times a week.
3. Support Gut Health:
Add fermented foods, prebiotic fibres or resistant starches to your every meal.
4. Stay Active:
Regular aerobic exercise increases the production of brain-derived neurotrophic factor (BDNF), supporting memory and learning.
5. Practice Mindful Eating:
Slow down, savour your food, and focus on hunger and fullness cues to reduce emotional eating.
Final Thoughts: Every Meal Shapes Your Mind
The evidence is clear: what you eat today shapes your brain's functioning tomorrow. High-fat, high-sugar diets can impair memory, focus, and emotional well-being in a matter of weeks, even if you’re young and healthy. But with conscious food choices and lifestyle changes, you can protect your hippocampus, sharpen your cognition, and build resilience for the long term.
Optimise your diet, nurture your gut, and move your body.
Your brain will thank you.
Source:
University of Sydney. High-fat, high-sugar diets impact cognitive function. Published in 17 April 2025: Tran, DMD. Double, KS. Johnston, IN. et al. (2025). Consumption of a diet high in fat and sugar is associated with worse spatial navigation ability in a virtual environment. International Journal of Obesity. doi:10.1038/s41366-025-01776-8
References:
Adjibade, M. Julia, C. Allès, B. et al. (2019). Prospective association between ultra-processed food consumption and incident depressive symptoms in the French NutriNet-Santé cohort. BMC Med. 17(1), 78. doi:10.1186/s12916-019-1312-y
Cryan, JF. O'Riordan, KJ. Cowan, CSM. et al. (2019). The microbiota-gut-brain axis. Physiological Reviews. 99(4), pp. 1877-2013. doi:10.1152/physrev.00018.2018
Sanchez O. (2025). From Gut Dysbiosis to Neurodegeneration: The Final Link in Obesity-Cognitive Difficulties. Nutrunity. Available at: https://www.nutrunity.com/updates/final-link-in-obesity-cognitive-decline
Texas Institute for Neurological Disorders. (2025). The Effects of a High Sugar Diet on the Brain. Available at: https://www.texasinstituteforneurologicaldisorders.com/uncategorized/effects-high-sugar-diet-brain [Last Accessed: May 2025]